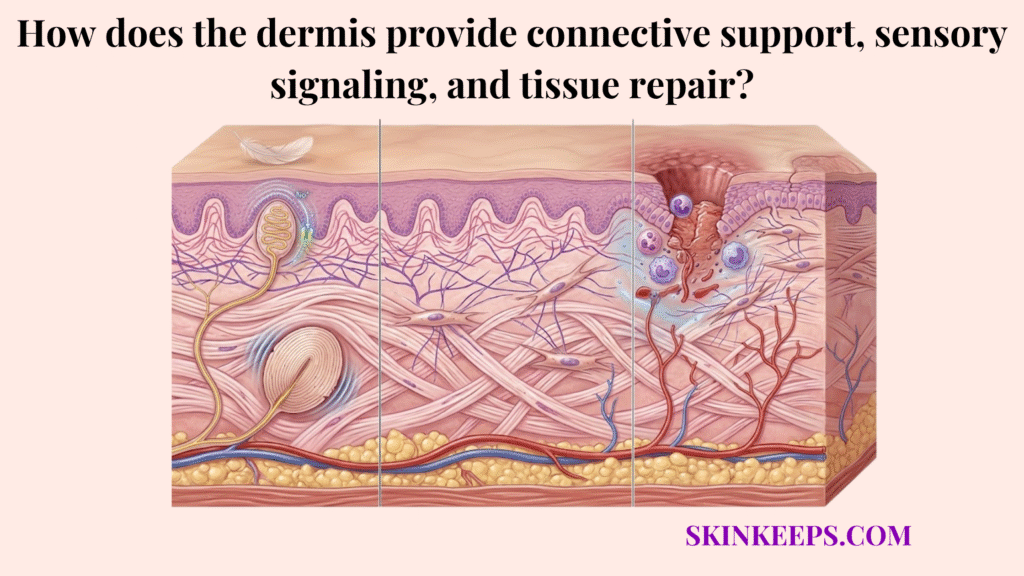
The dermis provides connective support, sensory signaling, and tissue repair by acting as the skin’s functional core layer, maintaining structural strength through collagen, enabling sensation through specialized nerve receptors, and driving wound healing through fibroblast activity. These functions directly influence visible skin health, and when they decline, the consequences often present as skin laxity, thinning, fragility, slower healing, altered sensitivity, and reduced bounce. The dermis is not merely a passive supporting layer; it operates as a highly active, functional biological system.
This biological system is built upon a distinct functional triad. Connective support maintains physical structure and recoil, sensory signaling detects critical environmental changes, and tissue repair restores the skin following an injury.
This guide explains exactly what the dermis is, how each of its three defining functions works, how to recognize when they are under strain, and how to support them with targeted, evidence-based care.
Quick Answers to Common Questions About the Dermis
To provide immediate clarity, this section answers the most common questions about the dermis using concise, clinically grounded explanations.
What is the dermis?
The dermis is the connective-tissue layer beneath the epidermis that gives skin much of its strength, elasticity, vascular support, and sensory responsiveness. It contains essential connective tissue, blood vessels, nerves, glands, and hair follicles within a highly functional biological network.
What does the dermis do?
The dermis defines deeper skin performance through three core functions: connective support, sensory signaling, and tissue repair. Noticeable skin laxity, unusually slower healing, and altered physical sensation often reflect accumulating structural stress within one of these vital functions.
What are the papillary and reticular dermis?
The dermis is organized into a papillary layer near the epidermis and a reticular layer deeper below, and each contributes differently to skin structure and responsiveness. The superficial papillary dermis handles fine vascular and sensory activity, while the deeper reticular layer provides robust structural density.
Why does the dermis matter in skin aging?
The dermis matters in skin aging because visible firmness, recoil, and repair quality depend heavily on the integrity of its connective matrix and fibroblast activity. As collagen production slows and extracellular components degrade, the skin physically loses its underlying structural strength.
How does the dermis help skin heal?
The dermis helps skin heal by coordinating inflammatory signaling, fibroblast activity, granulation tissue formation, collagen deposition, and later remodeling. True healing quality depends entirely on this highly organized internal repair process rather than simply achieving initial surface closure.
Can skincare support dermal function?
Skincare can support dermal function when it reduces cumulative UV stress, avoids repeated irritation, and uses evidence-based supportive care rather than cosmetic hype. However, topical regimens alone cannot substitute for medical care when underlying symptoms persist or become highly unusual.
When should someone seek medical review?
Medical review is appropriate when skin fragility, delayed healing, unusual pain, rapid worsening, or persistent inflammation extends beyond what gentle evidence-based care should reasonably improve. Seeking professional help ensures that underlying clinical conditions mimicking simple aging or sensitivity are properly addressed.
What is the dermis and how is it structured?
The dermis is the thickest and most functionally complex layer of the skin, situated beneath the epidermis and above the hypodermis, housing connective tissue, blood vessels, nerves, glands, and hair follicles.
Anatomically, the dermis is divided into two distinct regions: the papillary dermis and the reticular dermis. The papillary dermis is the thinner, upper region that interlocks directly with the epidermis to provide nutrients. The reticular dermis is the thicker, deeper region composed of dense, irregular connective tissue that anchors the skin and provides foundational durability.
These layers work together rather than independently to sustain skin vitality. The papillary dermis efficiently supports interface-level vascular and sensory activity, while the reticular dermis provides the denser structural support required for overall resilience. In fact, when asking which dermal layer contains dense collagen fibers, dermatologists point directly to this thick reticular foundation. The dermis varies in thickness across the body and is much thinner over the eyelids than over the back. The dermis is about 0.6 mm over the eyelids and about 4 mm over the back. [Cleveland Clinic, 2022]
- Papillary dermis → the upper interface that supports the epidermis and contains fine sensory and vascular structures
- Reticular dermis → the deeper structural zone with dense collagen, elastin, glands, and hair follicles
How does the dermis create connective support in the skin?
The dermis creates connective support in the skin through its extracellular matrix, a robust framework built by fibroblasts that dictates firmness, resilience, and visible aging.
The extracellular matrix functions practically as the skin’s physical scaffolding. It is not just inert filler tissue sitting between cells; it is the highly organized, dynamic framework that actively gives the dermis its structural coherence, enabling it to withstand physical stress and tension. To truly understand this mechanical strength, it is helpful to explore exactly where collagen and elastin are organized within the dermis.
This support relies on three primary components working seamlessly. Collagen forms the rigid pillars that resist pulling forces, elastin provides the coiled flexibility allowing the tissue to stretch, and glycosaminoglycan-rich hydration fills the spaces between these fibers to maintain essential volume. The specific mechanics of how elastin fibers are arranged in the dermal matrix directly determine the skin’s ability to snap back after being pinched or moved. Together, they connect back into one completely integrated support system.
- Collagen → provides tensile strength and helps prevent tearing or collapse
- Elastin → allows stretch and recoil so skin can return to shape
- Hyaluronic acid and other GAGs → attract and retain water for cushioning and plumpness
- Fibroblasts → maintain the matrix environment and support structural renewal
Key Takeaway: The dermis supports the skin by combining strength, elasticity, and hydration into one integrated connective system.
How does the dermal layer enable sensory signaling and environmental awareness?
The dermal layer enables sensory signaling and environmental awareness by housing specialized nerve structures that detect touch, pressure, vibration, temperature, and pain.
These specific nerve structures allow the body to respond quickly and appropriately to environmental change and potential injury. Without this rapid transmission of physical data, the skin would be entirely unable to protect itself from extreme heat or mechanical damage.
Proper sensory function depends fundamentally on both receptor integrity and surrounding dermal stability. When the tissue surrounding these nerves degrades, the physical transmission of signals can become altered, leading to changes in normal sensory awareness.
- Mechanoreceptors → detect touch, pressure, and vibration
- Thermoreceptors → detect heat and cold
- Nociceptors → detect pain and tissue damage
Key Takeaway: The dermal layer is not just structural. It is also a sensory interface that helps the body interpret and react to the environment.
How does the dermis drive wound healing and tissue repair?
When the skin barrier is breached, the dermis drives wound healing and tissue repair by coordinating a complex cascade of vascular constriction, inflammatory responses, and fibroblast activity to rebuild the tissue.
Healing quality depends entirely on efficient collagen synthesis, precise inflammation control, thorough tissue remodeling, and organized recovery rather than just rapid closure of the surface wound. Disrupted execution at any of these stages easily results in significant scarring or chronic, non-healing wounds.
As the wound progresses, fibroblasts quickly lay down granulation tissue—a temporary, highly vascularized matrix that fills the defect. However, this early repair tissue is significantly weaker than native skin and is not the same as fully remodeled strength. The inflammatory phase usually lasts several days, and the proliferative phase is characterized by granulation tissue formation, reepithelialization, and neovascularization and can last several weeks. [NCBI, 2023]
- Injury breaches the skin barrier
- Dermal blood vessels constrict and clot
- Inflammatory cells respond to damage
- Fibroblast activity supports connective rebuilding
- Granulation tissue forms
- New collagen matrix is synthesized
- Tissue remodels and strengthens over time
Key Takeaway: The dermis drives tissue repair by coordinating clotting, inflammation, fibroblast activity, and new matrix formation.
How can you tell if your dermis is weakening or damaged?
You can tell your dermis is weakening or damaged by observing distinct structural failures, such as slower wound healing, increased skin laxity, and fine lines becoming deeper or more persistent.
These clinical failures translate directly into noticeable daily reader experiences. The skin begins visibly sagging along the jawline, loses its youthful bounce when gently pinched, and tears much more easily when subjected to minor friction or accidental scrapes.
These patterns act as structural warning signs that the underlying tissue requires support, but they do not serve as formal self-diagnoses for medical connective tissue disorders.
- Slower wound healing
- Increased skin laxity or sagging
- Fine lines becoming deeper or more persistent
- Reduced elasticity or bounce
- Thinner, more fragile skin
- Changes in sensation, including numbness or increased sensitivity
Key Takeaway: These signs can reflect weakening connective support, reduced repair capacity, or impaired sensory function in the dermis.
When should you take action to protect or repair your dermis?
You should take action to protect or repair your dermis at the earliest signs of structural decline, as early intervention prevents cumulative matrix damage from progressing into advanced tissue fragility.
Early action remains vastly more realistic and effective than pursuing delayed correction once the matrix has fully collapsed. Preserving existing collagen networks yields superior structural results compared to attempting to rebuild entirely degraded dermal tissue later in life.
The stages of structural change serve as practical decision guidance to help map interventions, rather than functioning as strict diagnostic staging parameters.
Early-stage changes
- mild fine lines
- slight loss of elasticity
- small delays in healing
- early dullness or reduced bounce
Action: Begin consistent collagen-supportive and protective habits early.
Moderate-stage changes
- noticeable skin laxity
- slower recovery after irritation or injury
- more visible texture change
- persistent sensitivity or inflammation
Action: Combine topical support, lifestyle changes, and more targeted skin-repair strategies.
Advanced-stage changes
- deep wrinkling
- marked thinning or fragility
- chronic slow healing
- ongoing structural decline or sensory changes
Action: Consider professional evaluation and clinically guided treatment.
Key Takeaway: The best time to support the dermis is before structural loss becomes advanced, because early intervention is more effective than late correction.
What is the difference between a healthy dermis and a degraded dermal layer?
The primary difference between a healthy dermis and a degraded dermal layer lies in the density of its connective matrix, the responsiveness of its sensory signaling, and the efficiency of its wound-healing fibroblasts.
| Function | Healthy dermis | Degraded dermal layer | Visible symptoms |
|---|---|---|---|
| Connective support | Dense collagen, good elasticity, strong matrix hydration | Collagen loss, elastin fragmentation, reduced hydration | Wrinkles, sagging, thinning |
| Sensory signaling | Responsive nerve receptors and stable sensory awareness | Reduced or altered signaling | Numbness, irritation, abnormal sensitivity |
| Tissue repair | Efficient fibroblast activity and organized healing | Slower repair and weaker remodeling | Delayed healing, prolonged redness, scarring |
How can you protect and strengthen the dermis effectively?
You can protect and strengthen the dermis effectively by shifting from surface-level hydration to targeted strategies that stimulate connective support, protect sensory pathways, and improve natural healing.
Your chosen support strategy must accurately match the main biological function currently under strain. Applying topical moisturizers will not fix deep structural loss, and applying active collagen stimulators will not soothe disrupted sensory nerves.
The targeted actions below break down how to directly support the dermis’s connective, sensory, and repair mechanisms.
How can you stimulate connective support in the dermis?
You can stimulate connective support in the dermis by using evidence-based topical ingredients, such as retinoids and Vitamin C, that support collagen production and fibroblast activity.
These topical inputs perform best alongside highly supportive habits, including consistent photoprotection and deliberately avoiding repeated structural stress like aggressive friction. Protecting the matrix from preventable degradation is equally as important as attempting to stimulate new growth.
The ultimate goal remains structural support and preservation over time, rather than promising dramatic, overnight reversal of all established skin laxity.
How can you protect sensory function in the dermal layer?
You can protect sensory function in the dermal layer by reducing avoidable thermal and chemical injuries that disrupt the superficial nerve receptors located in the papillary dermis.
Protecting these pathways involves shielding the skin from repeated inflammatory damage and strictly limiting harsh scrubs, excessive heat exposure, and the stacking of acidic actives that significantly increase epidermal and dermal reactivity.
Sensory protection emphasizes strategic routine simplification and consistent trigger reduction rather than deploying aggressive corrective interventions that further overwhelm the sensory network.
How can you improve dermal healing and repair?
You can improve dermal healing and repair by maintaining a balanced, moist wound-healing environment that supports organized tissue recovery and reduces unnecessary disruption.
Proper repair explicitly requires avoiding behaviors that mechanically disrupt the delicate healing process, such as prematurely picking at the skin, stripping scabs, or repeatedly irritating compromised granulation tissue with strong topicals.
When basic supportive care is no longer enough to progress a wound through the normal healing phases, professional review becomes necessary to rule out deeper clinical complications.
What are the key functions of the dermis you need to remember?
The key functions of the dermis you need to remember are its ability to provide resilient connective support, enable rapid sensory signaling, and drive efficient tissue repair.
- The dermis provides structural support through collagen, elastin, and hydrated matrix components.
- It enables sensory signaling through specialized receptors and nerve structures.
- It drives tissue repair through fibroblast-led healing and matrix regeneration.
What can you do daily to support your dermal layer?
You can support your dermal layer daily by protecting it from preventable UV damage, using routines that stabilize collagen, and addressing signs of laxity before they progress.
- Protect the dermis from preventable damage, especially UV and repeated irritation
- Use a routine that supports collagen, hydration, and barrier stability
- Address early signs of thinning, laxity, or slow healing before they progress
Daily habits that protect structure, support repair, and reduce cumulative damage can help preserve dermal function over time. Consider a targeted skin-support plan or professional assessment if you are noticing increasing laxity, slow healing, or persistent signs of dermal decline.