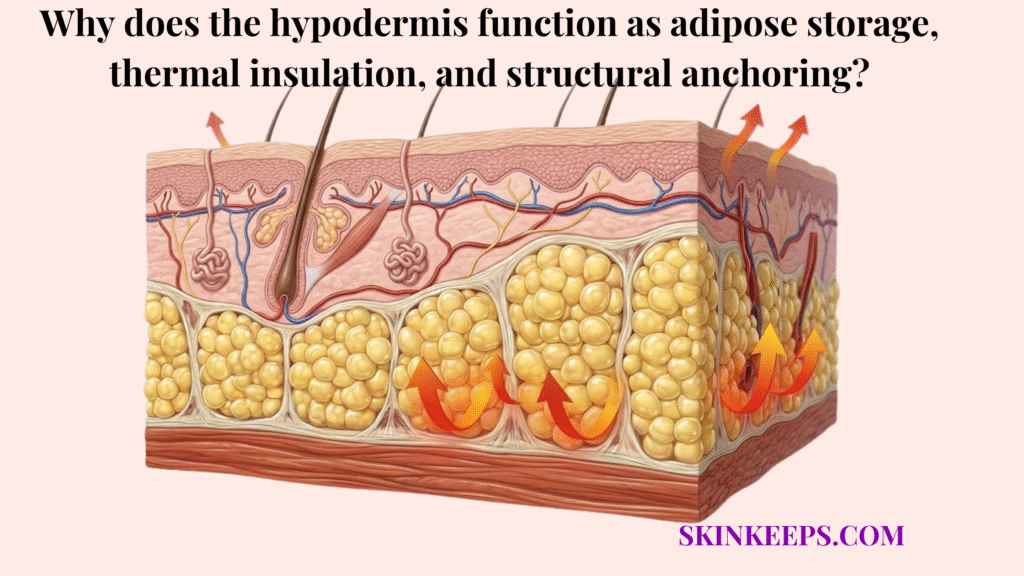
The hypodermis functions as adipose storage, thermal insulation, and structural anchoring because it is the body’s deepest support layer beneath the skin. It stores energy in adipocytes, helps preserve body heat through subcutaneous fat, and anchors the skin to deeper fascia and muscle through fibrous connective structures.
The hypodermis strongly affects visible volume, deep tissue cushioning, temperature regulation, and how securely the skin sits over deeper tissues. Thinning or degradation connects directly to visible hollowing, sagging, easy bruising, and increased cold sensitivity.
Understanding how the hypodermis works makes it easier to explain deep volume loss, thermal fragility, and structural sagging. The sections below break down its anatomy, core functions, warning signs of decline, when to act, and practical ways to protect or support this foundational layer.
Quick Answers to Common Questions About the Hypodermis
To provide immediate clarity, this section answers the most common questions about the hypodermis using concise, clinically grounded explanations.
What is the hypodermis?
The hypodermis is the deepest layer beneath the dermis, and it is commonly described as subcutaneous tissue. It forms the foundational base of the integumentary system, constructed primarily of adipose and connective tissues that anchor the upper skin layers to underlying fascia.
What does the hypodermis do?
The hypodermis supports the body through three core functions: adipose storage, thermal insulation, and structural anchoring. It effectively provides deep tissue cushioning, retains vital core body warmth, and acts as a mechanical buffer separating delicate skin from deep muscle movement.
Why is the hypodermis more than just fat?
The hypodermis is more than just fat because subcutaneous adipose tissue also behaves as a metabolically active endocrine organ. Adipocytes store metabolic energy while simultaneously secreting crucial signaling factors such as leptin and adiponectin to regulate systemic energy balance.
Why does thinning of the hypodermis matter?
Thinning of the hypodermis matters because less deep fat and connective support can reduce cushioning, weaken insulation, and make tissue contours look more hollow or deflated. This structural decline directly compromises visible volume and significantly increases susceptibility to deep tissue bruising.
What is the hypodermis and where is it located?
The hypodermis is the deepest layer beneath the dermis, and it forms the transition zone between the skin and the underlying fascia, muscle, and bone.
The hypodermis contains specialized adipose tissue, connective tissue bands, larger blood vessels, and nerve networks. This specific combination of fat lobules and fibrous septae constructs a highly organized matrix rather than a loose aggregation of random cells.
This layer functions strictly as the bridge between the skin and deeper support tissues. By integrating the overlying dermis into the deep muscular fascia below, the hypodermis guarantees that the entire cutaneous structure remains securely anchored while allowing necessary flexibility.
The hypodermis varies widely in thickness across the body. It may be less than 1 millimeter thick over the eyelids and external genitals, and more than 3 centimeters thick over the abdomen and buttocks. [Cleveland Clinic, 2021]
- Adipocyte lobules → clusters of fat cells that store energy and create volume
- Fibrous septae → connective bands that organize fat and help anchor tissue
- Macrovessels → larger blood vessels that supply deeper tissue
Why does the hypodermis function as the body’s primary adipose storage layer?
The hypodermis functions as the body’s primary adipose storage layer because it stores energy in adipocytes and acts as a reserve that can be mobilized when the body needs fuel.
Adipocytes efficiently store triglycerides, creating a dense reservoir of potential metabolic energy. This subcutaneous fat storage constitutes the largest reserve of lipid fuel available, allowing the body to sustain itself during periods of fasting or elevated physical demand.
When systemic energy is required, targeted hormonal signaling initiates lipolysis. This essential metabolic process breaks stored triglycerides down into free fatty acids and glycerol, releasing them from the adipose storage layer directly into the bloodstream for immediate cellular fuel.
Beyond acting as a passive fuel tank, the subcutaneous tissue actively monitors and communicates the body’s energy status. This dynamic shifts the layer’s role from simple deep tissue cushioning to complex systemic regulation.
By organizing fuel management and structural cushioning within the same biological compartment, the hypodermis perfectly integrates metabolic health with visible skin support.
How do adipocytes store energy in the hypodermis?
Adipocytes store energy in the hypodermis by holding triglycerides that can later be mobilized when the body requires additional fuel. Inside each fat cell, a large central lipid droplet securely isolates these triglycerides from the surrounding aqueous environment. This unique structure ensures the hypodermis acts as an incredibly stable deep energy reserve without disrupting the functional mechanics of the overlying dermis.
Why is the hypodermis more than just a fat layer?
The hypodermis is more than just a fat layer because subcutaneous adipose tissue also functions as an endocrine tissue involved in metabolic signaling. Adipose tissue actively secretes crucial signaling factors with systemic endocrine functions. By releasing specific hormones like leptin and adiponectin, the hypodermis continuously communicates energy status to the brain, influencing appetite, insulin sensitivity, and long-term metabolic balance. [Journal of Clinical Endocrinology & Metabolism, 2004]
- Energy reservoir → stores usable fuel for future energy needs
- Endocrine signaling → contributes to systemic metabolic communication
Key Takeaway: The hypodermis is not just passive padding. It is an active storage and signaling layer that influences both body contour and energy balance.
How does the subcutaneous tissue provide thermal insulation?
The subcutaneous tissue provides thermal insulation by acting as a fat-rich barrier that slows heat loss and helps preserve core temperature.
To fully grasp how hypodermal fat regulates body temperature, it helps to observe that this insulating function becomes vastly more important when the body is exposed to consistently cold environments. Without this protective adipose storage layer, the transfer of internal heat to the frigid external air would occur far too rapidly to sustain vital organ function.
Thermal insulation works perfectly alongside autonomic vasoconstriction to radically reduce peripheral heat loss. If you consider what role blood flow plays in hypodermal heat retention, the physiological process becomes clear: while blood vessels narrow to keep warm blood centralized, the thick layer of subcutaneous fat physically buffers the core against the outward escape of heat energy.
In direct tissue measurements, subcutaneous fat showed thermal conductivity of about 0.23 W/m·K, compared with about 0.46 W/m·K for muscle. The same study also reported lower thermal diffusivity in subcutaneous fat-containing tissue than in muscle. [PubMed, 2009]
- Environmental temperature drops
- Peripheral blood vessels constrict
- Subcutaneous fat reduces heat escape
- Core temperature is better preserved
Key Takeaway: The subcutaneous layer helps protect internal temperature by physically buffering the body against heat loss.
How does the hypodermis anchor and support the skin structurally?
The hypodermis anchors and supports the skin structurally by connecting it to deeper tissues while also providing cushioning, spacing, and movement support.
Fibrous septae create an organized, dense connective network straight through the adipose tissue. These structural bands help link the superficial dermis firmly to the much deeper, rigid support layers of muscle fascia.
By suspending the skin above the muscle, the interspersed adipose padding heavily absorbs pressure and helps the skin glide more smoothly over deeper structures during complex joint movements.
This distinct biomechanical architecture ensures that the skin remains securely attached without losing the crucial elasticity required for unhindered physical mobility.
What role do fibrous septae play in structural anchoring?
Fibrous septae play a structural anchoring role by connecting the skin to deeper tissues and organizing fat into supportive compartments. These tough connective bands create essential continuity between the superficial dermis and the deeper fascial support layers underneath. Because organization matters just as much as raw attachment, these septae arrange fat lobules into stable structural zones that resist gravitational pull and tissue collapse.
How does the hypodermis help the skin move without losing support?
The hypodermis helps the skin move without losing support by providing cushioning and spacing that allow smoother gliding over deeper structures. Tissue gliding is essential over joints and moving muscles. Deep tissue cushioning absorbs blunt forces and reduces friction, helping to prevent the skin from tearing or suffering unsupported mechanical collapse during rapid muscular contractions.
- Fibrous septae connect skin to deeper fascia
- Fat lobules provide padding and spacing
- Skin glides more smoothly over joints and moving structures
- Structural support helps resist sagging and tissue collapse
Key Takeaway: The hypodermis is part of the body’s deep support framework, not just a layer of stored fat.
How can you tell if your hypodermis is thinning or degrading?
You can tell your hypodermis is thinning or degrading when visible volume, cushioning, insulation, and deep structural support begin to decline.
These warning signs present visibly as distinct hollows under the eyes, flattening of the cheeks, or increased skin sagging around the jawline. Because deep tissue cushioning has depleted, the skin tears and bruises far more easily when bumping against solid surfaces.
Recognizing these patterns helps suggest reduced subcutaneous function rather than serving as a formal self-diagnosis for systemic metabolic disorders.
- Hollowing in the cheeks, temples, or under-eye area
- Increased skin sagging or a deflated appearance
- Easy bruising or reduced cushioning
- Feeling colder more often
- Greater tissue fragility in soft areas
Key Takeaway: These changes can reflect declining adipose volume, reduced insulation, or weakening structural support in the subcutaneous layer.
When should you take action to protect or restore your hypodermis?
You should take action to protect or restore your hypodermis at the first signs of deep tissue depletion, because early preservation is usually easier than late correction.
Preserving the remaining fat lobules and connective structures is practically far more realistic than attempting to reconstruct severely depleted subcutaneous tissue. Waiting for advanced depletion significantly limits the effectiveness of basic lifestyle interventions.
The two timing tiers below organize practical decision-making based on visual and physical markers of deep structural decline.
When do early-stage changes deserve action?
Early-stage changes deserve action when mild hollowing, slight laxity, rising cold sensitivity, or early loss of cushioning begin to appear. Addressing these early shifts stops rapid progression.
Action: Stabilize body weight, improve nutritional support, and avoid unnecessary fat depletion.
When do moderate or advanced changes need stronger intervention?
Moderate or advanced changes need stronger intervention when volume loss, sagging, bruising, or deep tissue depletion become clearly visible at rest. At this stage, the loss of structural anchoring is pronounced.
Action: Combine lifestyle support with targeted clinical strategies when needed.
Key Takeaway: Early preservation is usually easier than late correction, especially when deep support and fat volume have already declined.
What is the difference between a healthy hypodermis and a degraded subcutaneous layer?
The difference between a healthy hypodermis and a degraded subcutaneous layer lies in how well the tissue stores fat, preserves heat, and maintains deep structural support.
| Function | Healthy hypodermis | Degraded subcutaneous layer | Visible symptoms |
|---|---|---|---|
| Adipose storage | Stable fat volume and cushioning | Fat depletion or deflation | Hollowing, flattening |
| Thermal insulation | Better heat retention | Poor insulation | Cold sensitivity |
| Structural anchoring | Strong support and padding | Reduced deep support | Sagging, fragility, easier bruising |
These functional differences matter immensely because degraded structural anchoring causes overlying skin layers to sag, while a lack of stable fat volume eliminates the body’s mechanical shock absorption against daily trauma.
How can you protect and strengthen the hypodermis effectively?
You can protect and strengthen the hypodermis effectively by preserving adipose storage, supporting thermal buffering, and reinforcing the tissue’s deep structural framework.
A successful support strategy must align with the specific tissue function under strain. Because the hypodermis sits so deeply within the body, topical skincare cannot physically reach it; intervention requires internal and lifestyle stability.
The specific actions outlined below focus tightly on sustaining adipose storage, thermal insulation, and structural anchoring.
How can you preserve adipose storage in the hypodermis?
You can preserve adipose storage in the hypodermis by avoiding rapid depletion and maintaining more stable body-weight and nutritional patterns.
- Avoid repeated crash dieting or rapid weight cycling
- Maintain stable nutrition and body weight where possible
- Protect supportive fat pads from unnecessary depletion
Repeatedly starving and refilling adipocytes chemically destabilizes deep cushioning and permanently weakens connective septae.
How can you maintain thermal insulation in subcutaneous tissue?
You can maintain thermal insulation in subcutaneous tissue by supporting the metabolic and nutritional conditions that help preserve healthy fat buffering. Recognizing how hypodermal fat reduces heat loss from the body highlights exactly why maintaining this lipid layer is so crucial for daily comfort and structural health.
- Support overall metabolic and lipid health
- Avoid chronic under-fueling
- Include adequate dietary fat within a balanced eating pattern
Preserving robust fuel stores ensures the tissue remains capable of providing the necessary deep buffering against severe external temperature shifts.
How can you reinforce structural anchoring in the hypodermis?
You can reinforce structural anchoring in the hypodermis by supporting connective tissue integrity and reducing behaviors that accelerate deep tissue depletion.
- Support connective tissue health through overall nutrition
- Reduce behaviors that accelerate tissue depletion
- Consider clinically appropriate deep-support treatments when needed
Sustaining strong fibrous septae is the only biological way to prevent the overlying skin layer from completely succumbing to visible sagging and deep structural collapse.
What are the key functions of the hypodermis you need to remember?
The key functions of the hypodermis you need to remember are adipose storage, thermal insulation, and structural anchoring.
- The hypodermis stores energy through adipose tissue.
- It acts as a thermal barrier that helps preserve body heat.
- It anchors and cushions the skin through connective and fatty support structures.
All three functions work together continually; resilient structural anchoring requires stable fat volume, which in turn provides effective thermal insulation.
What can you do daily to support your subcutaneous tissue?
You can support your subcutaneous tissue daily by preserving stable fat volume, protecting deep cushioning, and avoiding patterns that accelerate tissue depletion.
- Maintain a stable body weight instead of repeated crash dieting
- Eat in a way that supports healthy fat and connective tissue maintenance
- Address early deep tissue loss before it becomes severe
Daily habits that preserve fat volume, thermal buffering, and deep structural support help protect the function of the hypodermis over time.
Consider a structured nutrition plan or a professional assessment if you are noticing visible hollowing, increased fragility, or deeper tissue sagging.