The skin microbiome supports epidermal defense by helping block pathogen overgrowth, strengthening local immune signaling, and maintaining a surface environment that favors barrier stability. Beneficial resident microbes act as part of the skin’s first-line defense by competing with harmful organisms and supporting protective responses in the epidermis. Reviews commonly describe the skin surface as carrying roughly 10^4 to 10^6 bacteria per square centimeter, which makes this microbial ecosystem biologically significant rather than incidental.
The epidermis is not protected by structure alone. Its defense also depends on a living microbial ecosystem that helps keep the barrier chemically, immunologically, and ecologically balanced. Reviews of skin microbiome biology consistently frame commensal communities as part of the first line of defense through direct competition, immune modulation, and support of the acidic skin surface.
Understanding how the skin microbiome supports epidermal defense makes it easier to explain why healthy skin resists pathogens more effectively, why over-stripping can backfire, and what actually helps preserve protective microbial balance.
Why is the skin microbiome important for epidermal defense?
The skin microbiome is important for epidermal defense because the epidermis is exposed constantly to environmental microbes, and many resident microbes help resist harmful invasion while supporting a more stable barrier environment.
Not all microbes on the skin are harmful. Many resident organisms contribute to defense by occupying ecological space, influencing local chemistry, and interacting with host immune pathways. This ensures the skin maintains its homeostatic balance.
The importance of the microbiome lies in the fact that the barrier must remain not only intact, but selectively hostile to pathogens and stable under constant exposure. Reviews consistently describe low skin pH and commensal occupancy as part of that first-line defense.
Where does the skin microbiome interact with the epidermis?
The skin microbiome interacts with the epidermis at and around the outer epidermal surface, where microbes meet the stratum corneum—the outer epidermal layer that interacts directly with the microbial environment—surface lipids, sweat-derived factors, and host defense molecules.
This interface is biologically active, not an inert dry wall, because microbial communities and host surface lipids—sebum- and barrier-related lipids that shape microbial habitat—continuously influence one another.
How does the skin microbiome prevent pathogen overgrowth on the epidermis?
The skin microbiome prevents pathogen overgrowth on the epidermis by occupying ecological space, competing for nutrients and attachment sites, and limiting the ability of harmful organisms to dominate the surface environment.
Competition matters because pathogens need space, nutrients, and access to establish overgrowth. By “crowding out” invaders, resident microbes—long-term commensal organisms that occupy the skin ecosystem—help defend the epidermis from infection.
How does the skin microbiome influence antimicrobial defense in the epidermis?
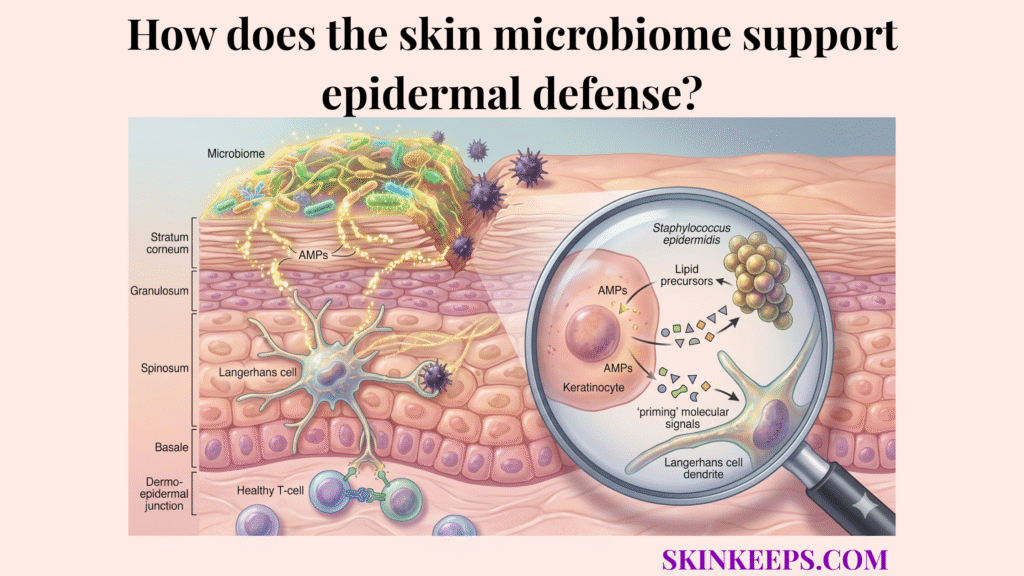
The skin microbiome influences antimicrobial defense in the epidermis by shaping surface conditions and directly enhancing antimicrobial peptides (AMPs)—host defense molecules that directly inhibit microbes—activity or induction in host cells.
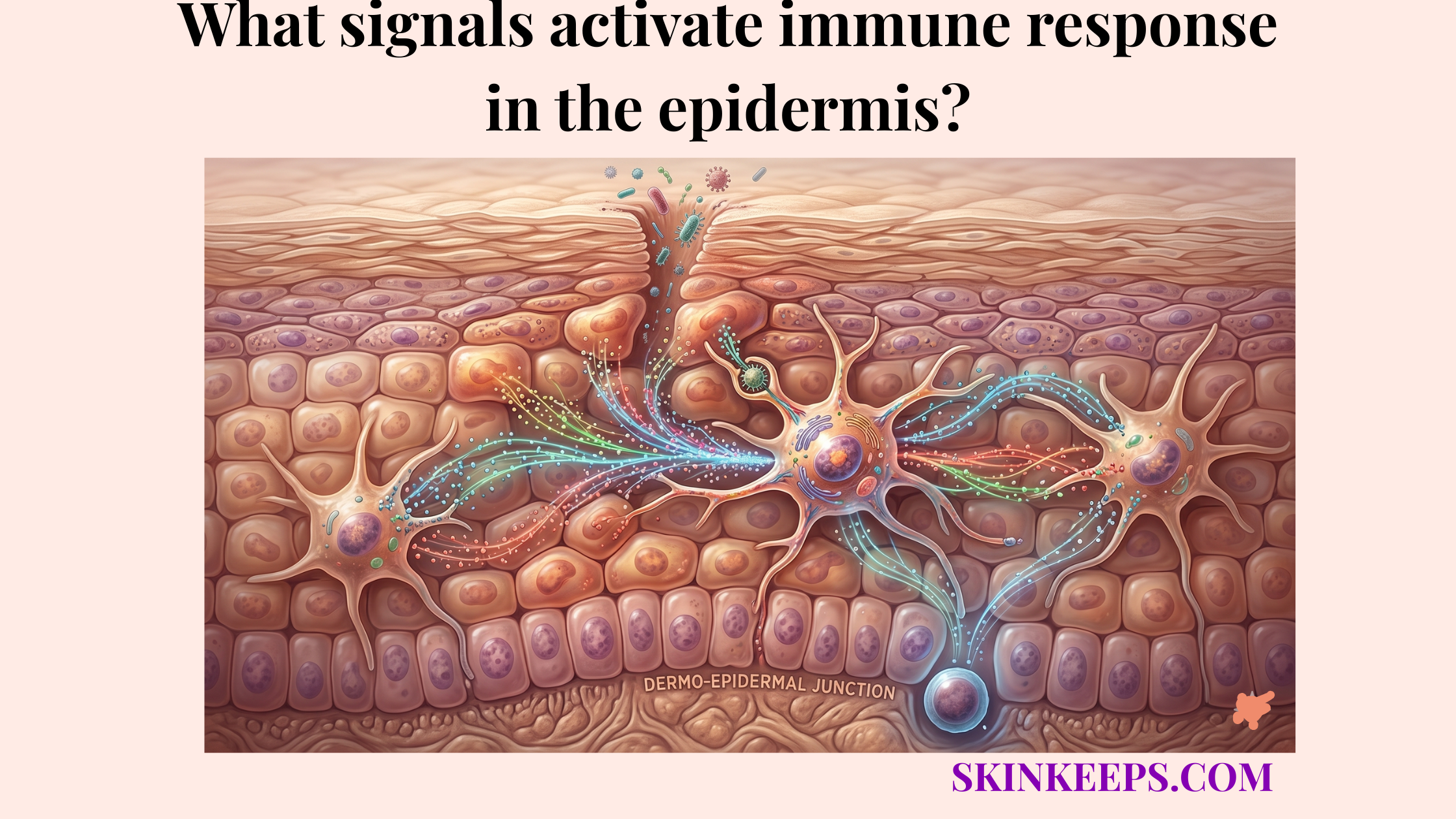
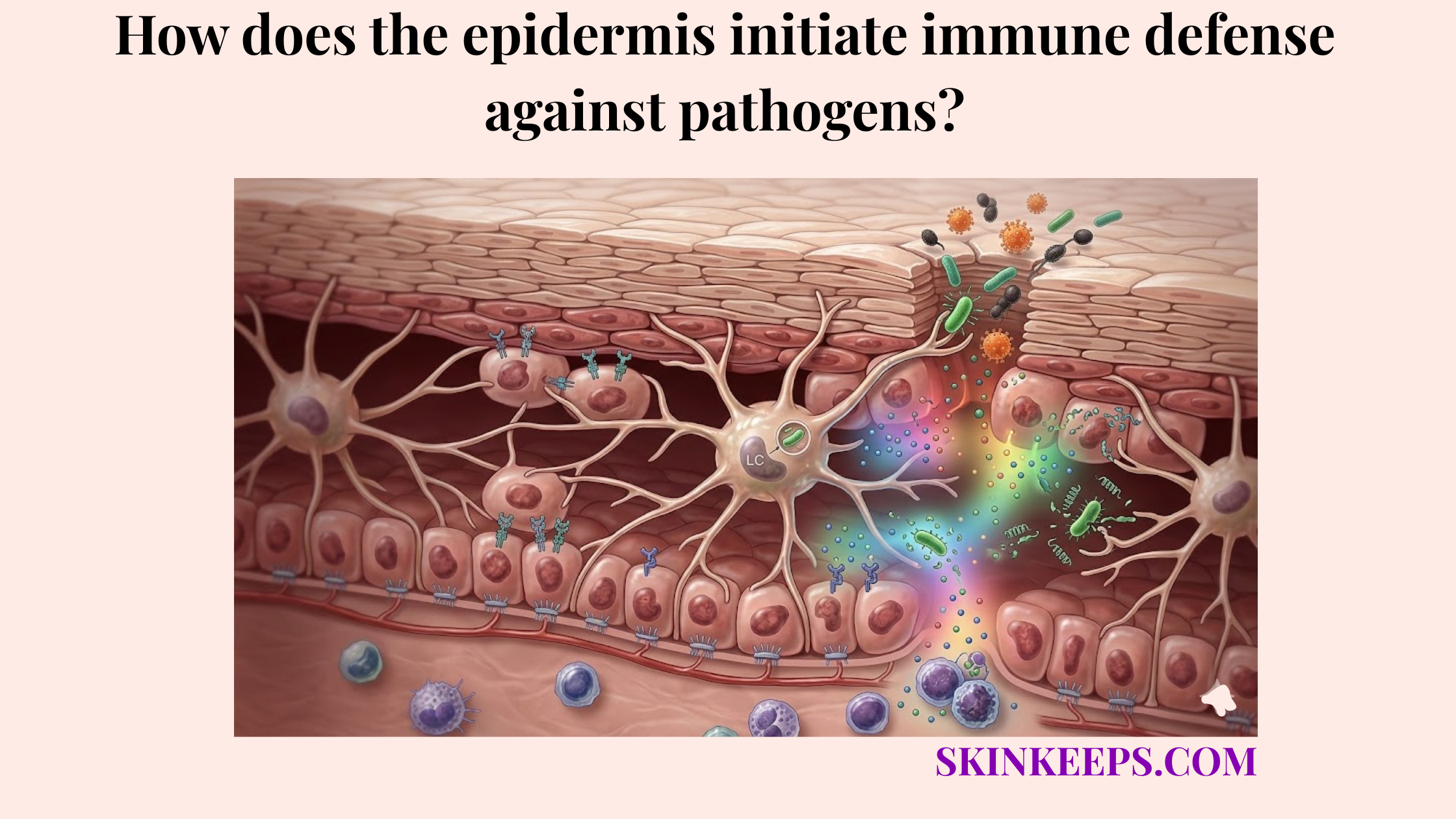
Beneficial resident microbes help ensure that the epidermis is ready to respond to threats. Primary studies show that Staphylococcus epidermidis–derived molecules can activate TLR2 signaling and induce AMP expression in keratinocytes, a key part of what signals activate immune response in the epidermis.
How does the skin microbiome help regulate epidermal immune signaling?
The skin microbiome helps regulate epidermal immune signaling by calibrating baseline immune readiness and reducing the likelihood that the epidermis drifts into either underreaction or chronic overreaction.
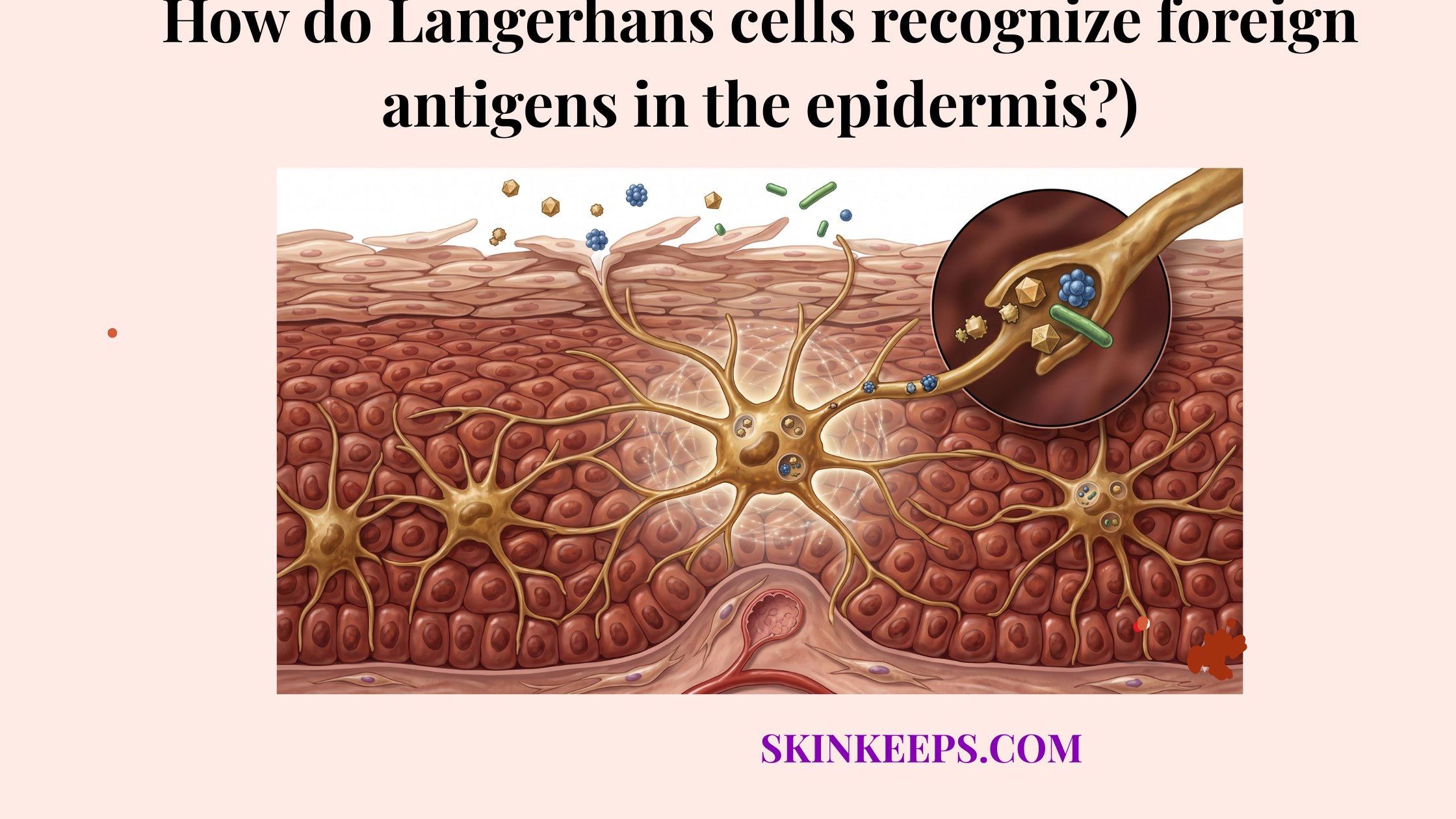
Microbial balance matters because resident exposure can train host defense pathways, whereas dysbiosis—disruption or imbalance in normal microbial ecology—can distort the tone of signaling. This training is essential for Langerhans cell surveillance.
How do resident microbes help calibrate immune readiness?
Resident microbes help calibrate immune readiness by maintaining a balanced baseline of epidermal vigilance that supports defense without requiring chronic inflammation. Lai et al. (2010) showed that specific commensal molecules can activate TLR2 signaling to increase antimicrobial peptide expression (PMC).
| Feature | Verified Figure | Significance for Defense |
|---|---|---|
| Skin bacterial density | ~10^4 to 10^6 bacteria/cm² | Abundant enough to influence host defense |
| Healthy skin surface pH | 4.1 to 5.8 | Acidic range helps restrain pathogens |
| AD S. aureus colonization | Often >90% | Dysbiosis coincides with weakened control |
How does the skin microbiome support barrier chemistry such as pH and surface lipids?
The skin microbiome supports barrier chemistry such as pH and surface lipids by helping maintain a surface environment that is less favorable to pathogen expansion and more favorable to normal barrier function.
Healthy skin surface pH is described as an acidic skin pH—the slightly acidic surface range (4.1 to 5.8)—which helps restrain pathogens such as S. aureus. This environment is critical for the prevention of transepidermal water loss (TEWL).
How does a balanced microbiome compare with dysbiosis in epidermal defense?
A balanced microbiome supports calmer, stronger epidermal defense, whereas dysbiosis weakens protection and makes the skin more reactive or inflammation-prone. Reviews of atopic dermatitis consistently describe microbial diversity loss and S. aureus expansion during flares.
| Microbiome state | Pathogen control | Immune signaling | Barrier effect |
|---|---|---|---|
| Balanced microbiome | Stronger control | Stable | Supported |
| Dysbiosis | Weaker control | Distorted | Less stable |
How can you tell when microbiome-supported epidermal defense is weakening?
When microbiome-supported epidermal defense is weakening, the skin often becomes more reactive, less resilient, and less able to maintain stable surface balance. Recurrent irritation and more frequent superficial infections fit the logic of reduced microbial support.
Warning Signs Checklist
What habits help support a healthy skin microbiome and stronger epidermal defense?
The best way to support a healthy skin microbiome and stronger epidermal defense is to protect the barrier environment that beneficial microbes need in order to function well.
How does gentler cleansing support the skin microbiome?
Gentler cleansing supports the skin microbiome by reducing unnecessary stripping of the surface conditions that resident microbes depend on. Walters et al. (2012) showed that surfactant-heavy cleansing can damage stratum corneum integrity, proving that gentle cleansing preserves the microbial habitat (PMC).
How does barrier support help maintain microbiome balance?
Barrier support helps maintain microbiome balance because a healthier barrier creates a more stable microbial habitat. Uberoi et al. (2021) showed that commensal microbiota regulate skin barrier function and repair through aryl hydrocarbon receptor signaling (PMC).
Problem: stripped, unstable, reactive skin
Implication: microbiome balance and epidermal defense may be weakening
Solution: cleanse gently, support the barrier, and reduce over-treatment
What are the key takeaways about how the skin microbiome supports epidermal defense?
- ● The microbiome defends the skin through competition and immune signaling.
- ● Balanced microbes are essential for a calm and resilient barrier.
- ● Support depends on gentle care and avoiding chronic surface disruption.
What daily steps can you take to support microbiome-based epidermal defense?
Microbiome Protection Protocol
Conclusively, healthy epidermal defense depends not only on what the skin blocks, but also on what it hosts. A stable microbiome helps the epidermis stay protective, balanced, and less vulnerable to disruption.