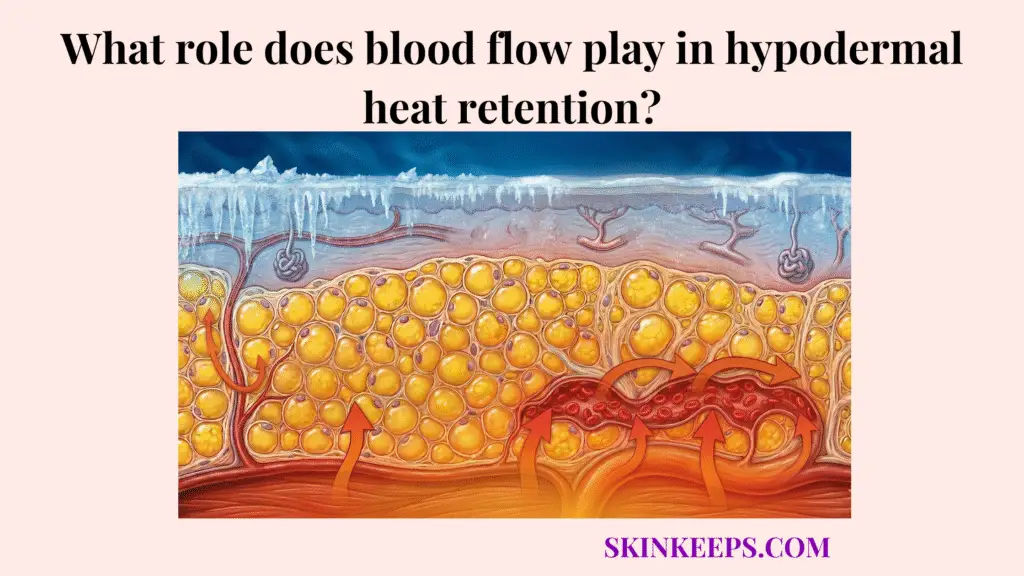
Blood flow plays a central role in hypodermal heat retention by controlling how much heat is carried toward the skin surface, where that heat can either be retained or lost to the external environment.
Blood flow does not work alone. It works together with how hypodermal fat reduces heat loss from the body, establishing a dynamic system where reduced blood flow usually improves heat retention while increased blood flow usually weakens it.
This article will explain why blood flow matters, what it means in this context, how the mechanism works beneath the skin, when reduced flow becomes protective, how increased flow changes heat escape, how blood flow compares with other mechanisms, and what limits it.
Why Blood Flow in Hypodermal Heat Retention Matters
Blood flow in hypodermal heat retention matters because it helps determine how much internal heat is delivered toward the skin surface, where that heat can either be conserved or lost.
Heat cannot escape efficiently unless it first physically reaches the superficial skin surface to meet the environment.
Blood flow is the major physiological mechanism controlling how much core warmth gets delivered to that critical boundary zone. Therefore, blood flow helps determine both active heat conservation and necessary heat release.
Why Blood Flow Helps Determine How Much Heat Reaches the Skin Surface
Blood flow helps determine how much heat reaches the skin surface because warm blood carries heat outward from deeper tissues toward the body boundary.
Blood operates as a primary transport route for thermal energy throughout the body, not just for oxygen and nutrients.
When more warm blood reaches the skin, vastly more heat becomes available near the surface. Surface heat availability is therefore one of the key determinants of heat retention versus heat loss. Johnson and Kellogg (2010) noted that cutaneous blood flow has a tremendous range, from nearly zero in extreme cold to about 7 L/min over the entire body surface when body temperatures are high [PMC].
Why Blood Flow Helps the Body Either Conserve or Release Heat
Blood flow helps the body either conserve or release heat because reduced flow lowers surface heat delivery, while increased flow raises it aggressively.
Reduced cutaneous blood flow means less internal heat is brought outward, directly supporting robust heat conservation.
Increased cutaneous blood flow means more heat is delivered toward the surface, where it can be lost much more easily. Blood flow serves as one of the body’s main adjustable levers for shifting between heat retention and heat release.
What Blood Flow in Hypodermal Heat Retention Means
Blood flow in hypodermal heat retention means the circulation-based control of how much heat is transported toward the subcutaneous and skin surface regions, where it can either be retained or lost.
This physiological concept defines the active transport of heat through the dynamic vascular network rather than the mere anatomical presence of blood vessels themselves. Assessing whether brown fat can generate heat within the hypodermis provides additional insight into active metabolic heat sources.
The focus remains specifically on how blood flow affects active heat retention and outward heat escape, rather than on all possible metabolic or nutritional functions of the skin.
How Blood Flow in Hypodermal Heat Retention Works Beneath the Skin
Blood flow in hypodermal heat retention works beneath the skin by influencing how much warm blood moves through vessels in and around the hypodermal region, changing local heat delivery and local heat retention.
Vascular networks located in and around the subcutaneous tissue actively dictate the exact local thermal state at any given moment.
Warm blood physically alters the baseline heat availability just beneath the skin. Vessel location and warm-blood movement together define the mechanics of this highly responsive heat-retention system.
How Blood Vessels in and Around the Hypodermis Influence Heat Movement
Blood vessels in and around the hypodermis influence heat movement by carrying warm blood into the tissue layers that lie extremely close to the body surface.
These local vessels completely shape how much intense warmth manages to reach the subcutaneous and skin-adjacent regions.
This continuous movement of warm blood radically changes the local thermal state beneath the skin. Vessel activity beneath the skin directly affects whether heat remains safely internal or becomes physically vulnerable to loss.
How Circulating Warm Blood Changes Local Heat Retention
Circulating warm blood changes local heat retention because the more warmth that arrives beneath the skin, the more heat can either be retained there or lost from there.
Blood flow physically alters the total amount of thermal energy actively present in local subcutaneous tissues.
Local heat retention improves significantly when this warmth is deliberately trapped and not rapidly passed onward to the superficial surface and environment. Blood flow successfully alters heat retention by actively altering the heat load present beneath the skin.
When Blood Flow in Hypodermal Heat Retention Decreases to Conserve Warmth
Blood flow in hypodermal Heat Retention decreases to conserve warmth when the body needs to reduce heat delivery to the skin surface, especially during cold exposure.
Reduced blood flow acts as an immediate and vital protective adjustment during freezing or cold conditions.
This reduced flow mechanically limits the total volume of heat brought toward the exposed surface layer. This protective vascular response is directly linked to intense vasoconstriction triggered by environmental cold exposure.
When Vasoconstriction Strengthens Blood Flow in Hypodermal Heat Retention
Vasoconstriction strengthens blood flow in hypodermal heat retention when narrowing skin vessels severely reduces warm blood delivery to the surface and thereby improves heat conservation.
Vasoconstriction operates as the primary vascular mechanism that heavily restricts surface-directed cutaneous blood flow.
Lower surface heat delivery guarantees that less thermal energy is available for outward passive loss. Vasoconstriction stands as one of the main physiological ways blood flow actively supports hypodermal heat retention.
When Cold Exposure Makes Reduced Blood Flow More Important
Cold exposure makes reduced blood flow more important because cold strongly increases the tendency for heat to leave the body, so lowering surface heat delivery becomes vastly more protective.
Colder environmental conditions establish a significantly stronger, unforgiving outward heat-loss gradient.
This hostile gradient exponentially increases the biological importance of reducing blood flow to the skin. Reduced cutaneous flow matters most when the environment strongly and constantly favors rapid heat escape.
How Reduced Blood Flow in Hypodermal Heat Retention Limits Heat Loss
Reduced blood flow in hypodermal heat retention limits heat loss by aggressively decreasing the amount of warm blood that reaches the skin surface, leaving less heat available to escape outward.
Reduced cutaneous blood flow functions strictly as a primary, immediate biological heat-conservation strategy.
The mechanism works effectively by forcefully lowering heat delivery to the boundary layer, not by increasing the physical thickness of structural insulation directly. Reduced flow links inextricably to the stronger retention of vital internal core warmth.
How Increased Blood Flow in Hypodermal Heat Retention Changes Heat Escape
Increased blood flow in hypodermal heat retention changes heat escape by rapidly moving more warm blood toward the skin surface, where that heat becomes incredibly easy to lose.
Increased skin blood flow aggressively raises the total amount of thermal energy pooling near the superficial skin surface.
This vascular flooding makes outward heat loss much more likely and efficient. Increased surface heat delivery and correspondingly weaker hypodermal heat retention represent the two main physiological results of this vascular change.
How Increased Blood Flow Moves More Heat Toward the Body Surface
Increased blood flow moves more heat toward the body surface by transporting significantly larger volumes of warm blood directly into superficial tissues.
More cutaneous flow means substantially more transported warmth, not merely a faster, unchanged circulation velocity.
The skin and subcutaneous surface zone become thermally richer and hotter when more warm blood arrives. Greater surface heat delivery is the main reason increased blood flow ultimately weakens heat retention. Chou et al. (2022) reported that in severe heat stress, skin blood flow may massively increase to about 7–8 L/min, which can represent roughly 50–60% of total cardiac output during supine rest [PMC].
How Greater Surface Heat Delivery Weakens Hypodermal Heat Retention
Greater surface heat delivery weakens hypodermal heat retention because more warmth arriving at the body boundary simply means more heat is available to easily escape to the environment.
Internal body heat must be positioned physically near the body surface before it can be lost efficiently to the surrounding air.
Greater blood-driven surface warming therefore drastically weakens thermal retention. Increased blood flow is highly useful for emergency heat release, but incredibly detrimental for conserving necessary warmth.
Why Blood Flow in Hypodermal Heat Retention Works With Hypodermal Fat Insulation
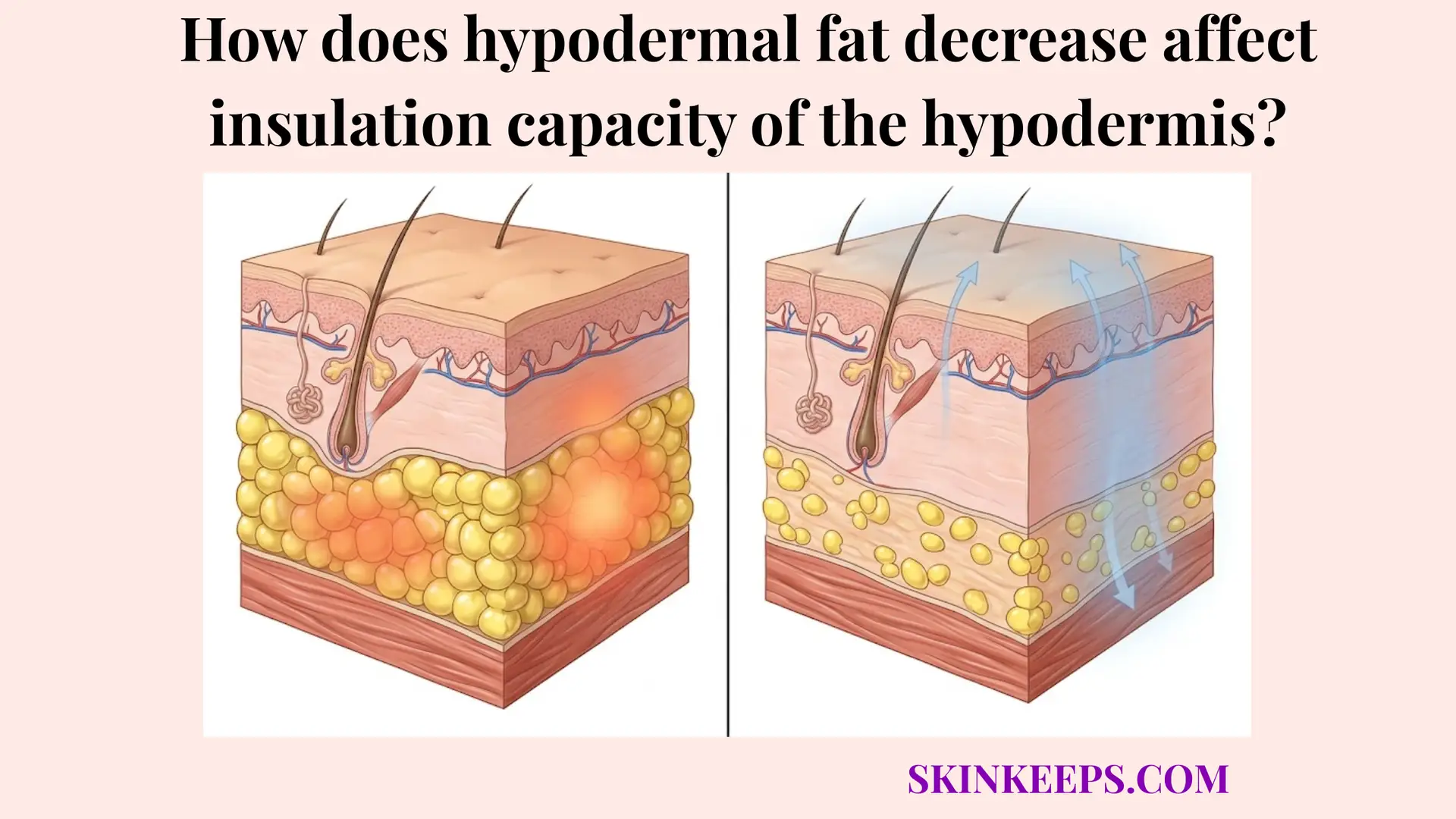
Blood flow in hypodermal heat retention works with hypodermal fat insulation because circulation actively controls how much heat reaches the subcutaneous-surface zone, while fat insulation helps physically resist how easily that delivered heat escapes.
Cutaneous blood flow and subcutaneous insulation function together as complementary, entirely synergistic, rather than competing, physiological mechanisms.
Blood flow determines active surface heat availability, while fat dictates the passive physical resistance to outward thermal transfer. Combined protection is significantly stronger and more thermally stable than either mechanism acting alone.
Why Blood Flow Control and Fat Insulation Protect Heat More Effectively Together
Blood flow control and fat insulation protect heat more effectively together because reduced surface heat delivery and increased physical resistance to outward transfer perfectly reinforce one another.
On the circulation side, restricted blood flow means far less internal heat ever manages to reach the vulnerable surface boundary.
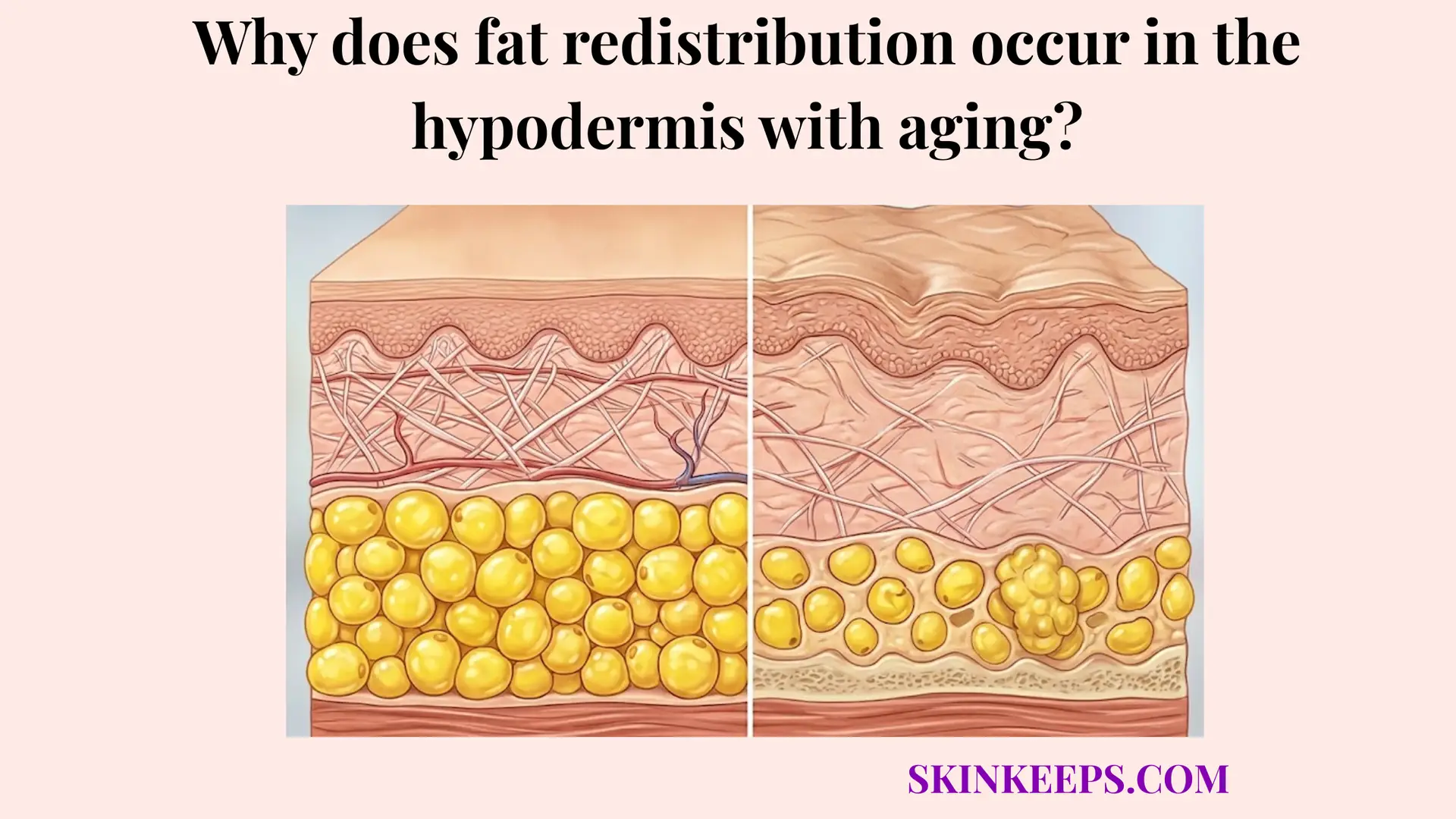
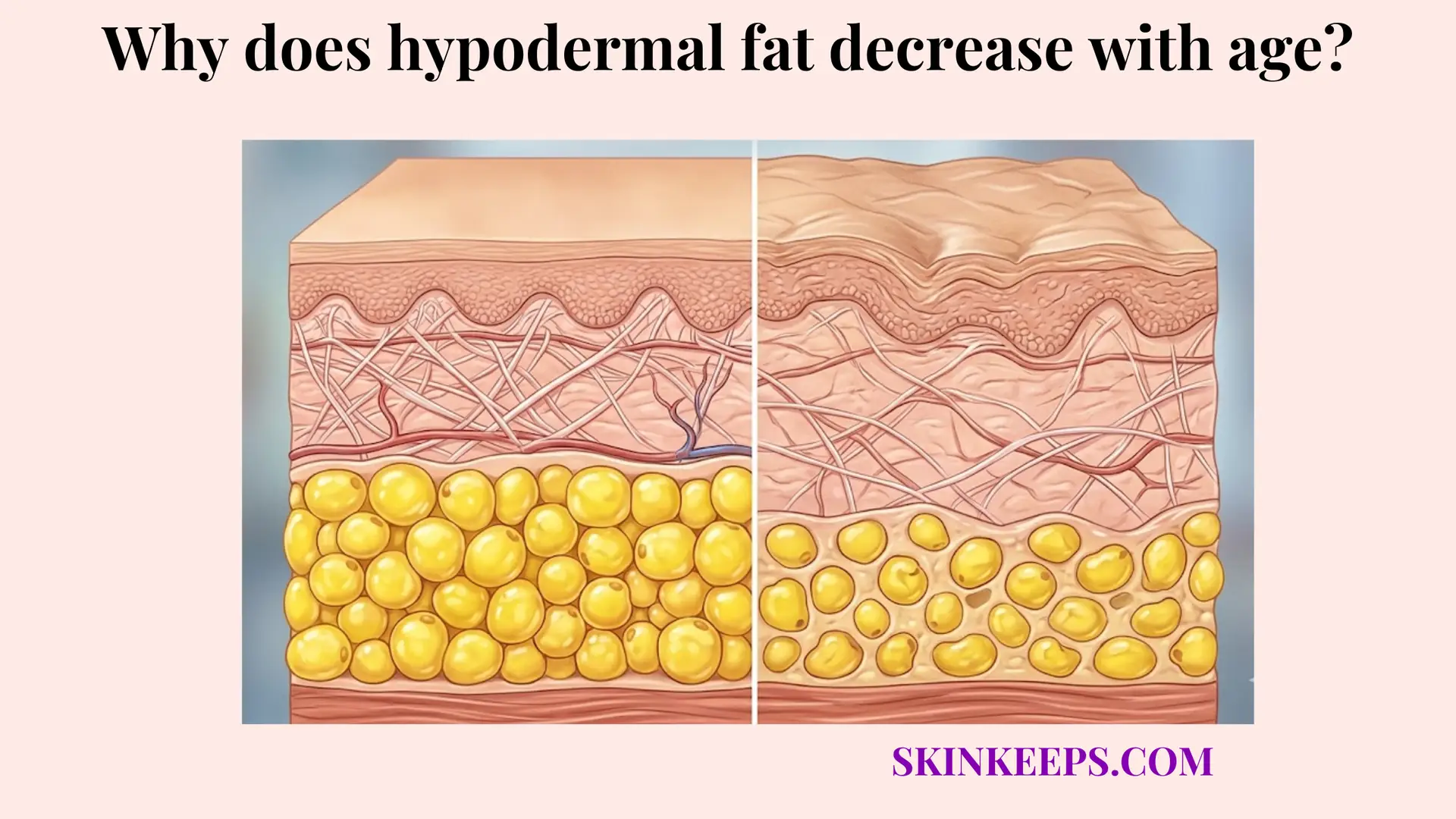
On the insulation side, thick subcutaneous fat strongly resists the outward transfer of whatever small amount of heat does arrive. Exploring why hypodermal fat decreases with age reveals that blood flow must compensate when structural fat is lost. Combined physiological control creates vastly stronger heat retention than either mechanism operating alone in a vacuum.
How Blood Flow in Hypodermal Heat Retention Differs From Insulation Alone
Blood flow in hypodermal heat retention differs from insulation alone because circulation changes heat delivery rapidly and dynamically, while insulation mainly changes static, passive resistance to heat escape.
Subcutaneous fat insulation remains mostly a passive, static, and slowly changing structural barrier against heat transfer. Speakman and Westerterp (2018) highlighted that higher adiposity can improve cold insulation but impede heat loss, showing that static insulation requires dynamic blood flow to manage complex thermal changes [PubMed].
Cutaneous blood flow, however, is highly dynamic and actively adjustable from minute to minute. Heat retention depends completely on both the active amount of heat delivered and the passive structural resistance to losing it.
Which Factors Affect Blood Flow in Hypodermal Heat Retention
Several factors affect blood flow in hypodermal heat retention, especially environmental temperature, vasomotor responses, body region, chronological age, metabolism, and physical activity level.
Environmental temperature and internal vasomotor control act as the main immediate, real-time regulators of the entire vascular system.
Regional differences, age-related vascular changes, metabolic conditions, and physical activity levels also strongly and predictably influence the final outcome. Blood-flow-driven heat retention is highly context-dependent rather than a rigidly fixed biological constant.
Which Roles Temperature, Vasomotor Responses, and Body Region Play in Hypodermal Heat Retention
Temperature, vasomotor responses, and body region affect hypodermal heat retention by changing exactly how much warm blood is delivered to different skin areas under distinctly different thermal conditions.
Extreme cold and intense heat shift peripheral blood flow in entirely different, opposite directions.
Vasoconstriction and vasodilation directly alter local heat delivery, while different body regions show different heat-retention behavior simply because vascular networks are not uniformly distributed across human anatomy.
Which Roles Age, Metabolism, and Activity Level Play in Hypodermal Heat Retention
Age, metabolism, and activity level affect hypodermal heat retention because they drastically change circulatory responsiveness, baseline heat production, and the body’s urgent need to either conserve or release warmth.
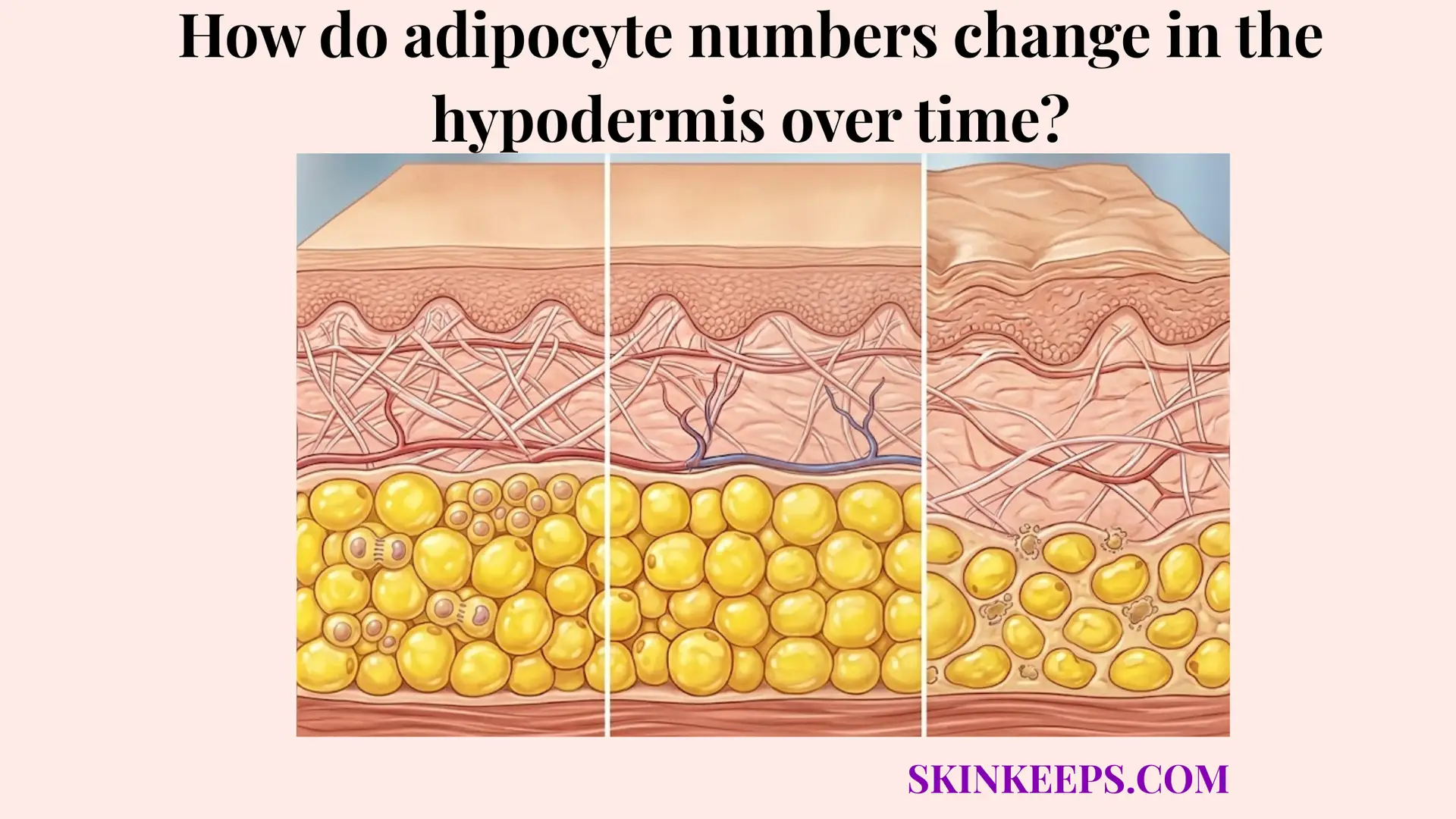
Advanced age can systematically reduce general thermoregulatory vascular responsiveness, making overall retention less efficient. This decline mirrors how adipocyte numbers change over time.
Metabolism and physical activity drastically alter internal heat production and thereby alter how much active retention is actually needed. Blood-flow effects on heat retention cannot be fully understood without considering this broader physiologic and energetic context.
How Blood Flow in Hypodermal Heat Retention Compares With Other Heat-Conservation Mechanisms
Blood flow in hypodermal heat retention differs from other heat-conservation mechanisms because it exclusively controls heat delivery to the surface, while mechanisms like fat thickness, shivering, and metabolic heat production affect retained warmth through entirely other biological routes.
The special role of blood flow centers exclusively on dynamically altering how much heat reaches the vulnerable skin boundary.
This contrasts sharply with static structural insulation or active muscular heat-generation mechanisms. Effective, robust cold defense depends absolutely on all of these diverse mechanisms working flawlessly together.
How Blood Flow in Hypodermal Heat Retention Compares With Hypodermal Fat Thickness
Blood flow in hypodermal heat retention compares with hypodermal fat thickness in that blood flow changes heat delivery rapidly and dynamically, while fat thickness changes passive insulation structurally.
Cutaneous blood flow represents the dynamic, rapidly shifting nature of real-time thermal vascular control.
Hypodermal fat thickness represents the static, long-term structural nature of anatomical thermal resistance. Complete heat retention depends strictly on both dynamic heat delivery and structural heat-loss resistance.
How Blood Flow in Hypodermal Heat Retention Compares With Shivering and Metabolic Heat Production
Blood flow in hypodermal heat retention compares with shivering and metabolic heat production in that blood flow strictly controls heat conservation at the body surface, while shivering and metabolism actively increase the internal heat supply.
Blood flow directly affects whether existing internal heat manages to reach the exposed surface and escape.
Shivering and metabolic activity affect exactly how much total heat exists in the core to be retained. Cutaneous circulation flawlessly conserves thermal energy, while cellular metabolism actively produces it.
When Blood Flow in Hypodermal Heat Retention Is Not Enough on Its Own
Blood flow in hypodermal heat retention is not enough on its own when severe external cold, weak anatomical insulation, or limited physiologic reserve make surface heat control completely insufficient by itself.
Blood-flow control alone cannot fully guarantee core warmth or survival during severe, prolonged environmental exposure.
Subcutaneous fat insulation, vigorous shivering, highly protective clothing, and safe shelter may still be absolutely necessary to prevent hypothermia. Cutaneous circulation remains a major mechanism, but it is not the entire heat-retention system.
How Regional Blood Flow Changes Hypodermal Heat Retention Across the Body
Regional blood flow changes hypodermal heat retention across the body because different body areas simply do not receive identical cutaneous blood flow under the exact same thermal conditions.
Biological heat retention is completely not spatially uniform across the entire human body.
Some peripheral regions may deliver or conserve heat entirely differently depending solely on their local vascular density. Regional cutaneous blood flow directly and predictably contributes to regional differences in retained warmth and local heat loss.
Which Key Takeaways Define Blood Flow in Hypodermal Heat Retention
The key takeaways are that blood flow controls how much heat reaches the skin surface, reduced blood flow usually supports heat retention, increased blood flow usually weakens heat retention, and blood flow works perfectly together with hypodermal fat insulation rather than replacing it.
Cutaneous blood flow and subcutaneous fat insulation successfully operate as a unified, tightly complementary defensive system.
Blood flow remains thoroughly central to temperature control, but it does not represent the entire, foolproof biological heat-retention system on its own.
How Blood Flow Affects Hypodermal Heat Retention
| Blood flow state | What happens in the vessels | Effect on heat retention | Effect on heat loss |
|---|---|---|---|
| Reduced | Less warm blood reaches the surface | Heat retention strengthens | Heat loss falls |
| Normal | Usual surface heat delivery continues | Baseline retention | Baseline heat loss |
| Increased | More warm blood reaches the surface | Heat retention weakens | Heat loss rises |
Comparison: Reduced vs Normal vs Increased Blood Flow
| Blood flow level | Heat delivery to surface | Heat retention strength | Heat loss tendency | Typical condition |
|---|---|---|---|---|
| Reduced | Lower | Stronger | Lower | Cold exposure, vasoconstriction |
| Normal | Baseline | Moderate | Baseline | Neutral conditions |
| Increased | Higher | Weaker | Higher | Heat exposure, vasodilation |
Final Heat-Retention Checklist
Quick Answers About Blood Flow in Hypodermal Heat Retention
Does more blood flow improve heat retention?
No. More cutaneous blood flow actually weakens heat retention because it aggressively transports internal core warmth to the superficial skin surface, where it is rapidly lost to the environment.
Why does reduced skin blood flow help conserve warmth?
Reduced skin blood flow conserves warmth because extreme vasoconstriction locks warm blood deep inside the body core. By starving the skin surface of blood, less heat becomes available to escape outward.
How does blood flow work with hypodermal fat?
Skin blood flow controls how much heat is actively delivered to the surface boundary, while hypodermal fat acts as a physical structural barrier that passively resists the escape of whatever heat arrives there.
Why is blood flow important during cold exposure?
During cold exposure, the environment strongly pulls heat away from the skin. Reducing blood flow to the surface is the body’s fastest, most effective defense for keeping core heat safely insulated.
Can blood flow alone prevent heat loss?
No. While restricting blood flow reduces heat delivery to the surface, complete protection requires subcutaneous fat insulation, shivering for heat production, and appropriate external clothing in severe conditions.
Does regional circulation change local heat retention?
Yes. Regional circulation varies drastically across the body. Areas with dense vascular networks, like the hands and face, can lose or retain heat very differently than heavily insulated regions like the torso.
How is blood flow different from shivering?
Blood flow control is a heat-conservation mechanism that changes how existing heat is distributed. Shivering is an active heat-production mechanism that forces muscles to generate entirely new thermal energy.
How is blood flow different from fat insulation?
Blood flow is highly dynamic and changes from minute to minute based on thermal needs. Hypodermal fat insulation is structural, providing a constant, passive baseline resistance to heat movement.
Conclusion
Blood flow plays a central role in hypodermal heat retention because it controls how much warm blood carries heat toward the skin surface, where that heat can either be retained or lost.
Reduced cutaneous blood flow intensely and dependably supports vital heat retention, while increased cutaneous blood flow aggressively supports rapid heat release.
Cutaneous blood flow ultimately remains a major, highly dynamic component of the hypodermal heat-retention system, but it relies wholly on structural insulation and systemic health to achieve maximum thermal defense.