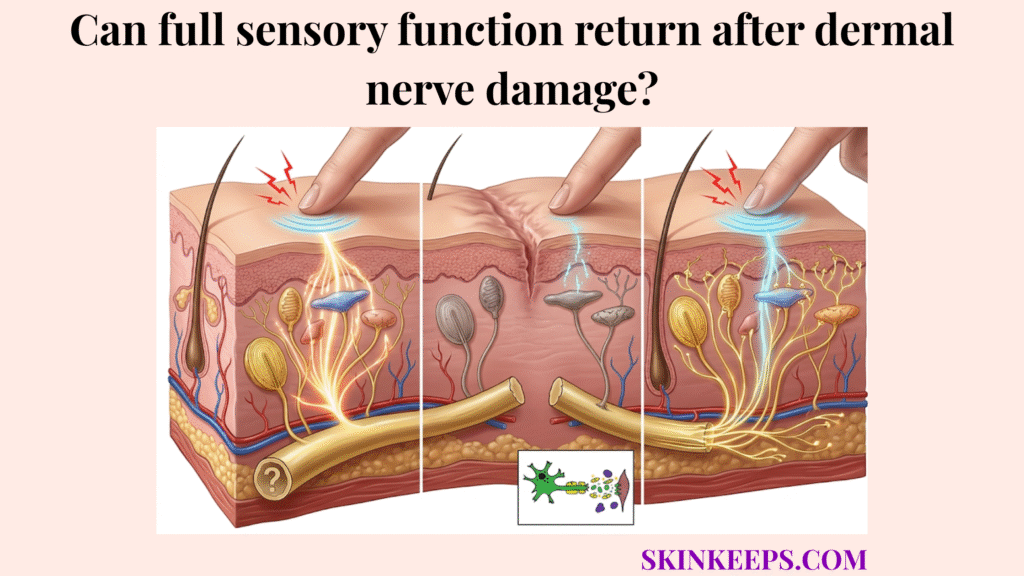
Full sensory function can return after dermal nerve damage, but it depends on whether the regenerating nerve reconnects accurately, travels the correct distance successfully, and heals in a supportive tissue environment.
Numbness, tingling, hypersensitivity, or altered touch can persist even when the skin looks completely healed, because regenerating the outer barrier is structurally different from rebuilding a delicate neural network. A closed wound does not automatically mean a fully rewired sensory map.
Understanding the factors and probability of sensory return requires mapping the biological baseline, exploring topographic precision, comparing injury types, tracking Schwann-cell guidance, factoring in recovery distance, and applying sensory re-education alongside practical optimization strategies.
What is the biological baseline for whether full sensory function returns after nerve damage?
The biological baseline for whether full sensory function returns after nerve damage is that regrowth alone is not enough; the regenerating axon must also reinnervate the correct target accurately enough for meaningful sensory function to re-emerge.
Understanding how dermal nerves regenerate after injury reveals that structural regrowth simply means a nerve fiber has extended forward into the healing wound. Functional sensory restoration, however, requires target reinnervation, the successful, functional reconnection of regrowing nerve fibers with their specific original sensory receptors in the skin.
If the brain receives mismatched input from a sensory nerve that randomly wired itself to the wrong receptor, the resulting feeling will be incomplete, numb, or severely distorted, completely limiting true functional recovery.
Grinsell and Keating (2014) note in a review of peripheral nerve reconstruction that less than half of patients who undergo severe nerve repair regain good to excellent motor or sensory function, which is one of the clearest clinical reminders that while full recovery is possible, it is never guaranteed [PMC].
How does topographic precision determine whether full sensory function returns after nerve damage?
Topographic precision determines whether full sensory function returns after nerve damage because regenerating axons must reconnect to the appropriate original target or a functionally acceptable equivalent, not just to any available pathway.
Topographic precision ensures that a nerve fiber originally dedicated to a specific fingertip touch receptor finds its exact way back to that specific receptor type, rather than accidentally linking to a deep-pressure or pain sensor.
Structurally “successful” regeneration can still feel highly abnormal if targeting is imprecise. Misdirected regeneration leads directly to scrambled sensation, hypersensitivity, or distorted touch, proving that accurate reinnervation determines sensory recovery quality far more than raw axonal length.
How does injury type dictate if full sensory function returns after nerve damage?
Injury type dictates if full sensory function returns after nerve damage because the more intact the original guidance architecture remains, the greater the chance that regenerating axons can reconnect accurately.
Neurapraxia is a mild nerve injury with preserved axonal continuity. Because the internal connective tubes remain perfectly intact, the nerve only needs to recover its signaling function locally, making the probability of full, perfect return extremely high.
Axonotmesis involves actual axon damage but preserves the outer nerve sheaths, allowing for guided, though delayed, structural recovery. Neurotmesis is complete nerve transection where all guidance architecture is severed, resulting in a drastically lower chance of accurate reinnervation without surgical alignment.
Cuello et al. (2023) indicate that neurapraxia often resolves within 2–3 months with full recovery [StatPearls], while Althagafi and Nadi (2023) confirm that complete transection (neurotmesis) causes complete sensory loss and requires highly demanding surgical repair conditions for any meaningful functional sensory return [StatPearls].
How do Schwann cells support whether full sensory function returns after nerve damage?
Schwann cells support whether full sensory function returns after nerve damage by preserving the regeneration pathway, producing guidance signals, and helping regenerating axons find a route back toward useful targets.
Following injury, these specialized peripheral glial cells transform radically into repair Schwann cells. They line up end-to-end to form physical biological tubes that insulate and aggressively direct the advancing growth cone—the highly sensitive, searching tip of the regenerating axon.
This endoneurial tube support ensures that the regenerating fiber receives constant chemical and structural directional cues. Because Schwann cells guide sensory reconnection, they actively prevent the nerve from wandering aimlessly into scar tissue, drastically improving the chance of topographic precision.
How does recovery distance affect whether full sensory function returns after nerve damage?
Recovery distance affects whether full sensory function returns after nerve damage because longer regrowth paths require more time, more precision, and more sustained biological support, which increases the chance of stalling or incomplete reconnection.
Even when regeneration initiates perfectly, a massive anatomical distance magnifies the ongoing opportunity for error, pathway misdirection, and dense scar-tissue obstruction. The longer the journey, the more likely the growth cone will fail to maintain topographic precision.
The regeneration rate of dermal nerve fibers is commonly anchored by a practical clinical rule of about 1 mm per day. Consequently, longer reinnervation distances quickly become months-long (or years-long) recovery problems, guaranteeing delayed sensory return after skin healing is long finished. Althagafi and Nadi (2023) note that recovery can be poor when the target is simply too far away to be reinnervated within a biologically useful timeframe [StatPearls].
How do age and metabolic health affect whether full sensory function returns after nerve damage?
Age and metabolic health affect whether full sensory function returns after nerve damage because regenerative efficiency depends heavily on tissue quality, vascular support, Schwann-cell function, and the broader metabolic environment.
Younger, metabolically stable tissue naturally provides superior regenerative efficiency, yielding a decidedly higher probability of complete functional sensory return with fewer biological constraints.
Conversely, poor metabolic health, classically demonstrated by diabetic neuropathy, establishes severe microvascular and energy barriers. Microvascular support is non-negotiable for delivering the massive amounts of cellular fuel required to keep the growth cone advancing through damaged tissue.
| Recovery Variable | Effect on Precision | Probability of Full Return | Main Obstacle |
|---|---|---|---|
| Younger age | Better regenerative efficiency | Higher | Fewer biological constraints |
| Older age | Slower and less precise repair | Lower | Reduced regenerative capacity |
| Good metabolic health | Better support for regrowth | Higher | Fewer vascular and energy barriers |
| Poor metabolic health | More stalled or incomplete healing | Lower | Blood sugar, circulation, and tissue stress |
How does sensory re-education improve the chance that full sensory function returns after nerve damage?
Sensory re-education improves the chance that full sensory function returns after nerve damage because functional recovery depends not only on peripheral reconnection but also on the brain’s ability to interpret the returning signals accurately.
Sensory re-education is a structured cognitive and physical rehabilitation protocol designed to help the nervous system actively relearn and map altered sensory input following peripheral nerve repair.
Because peripheral regrowth is rarely perfect, sensation often returns in a scrambled, hypersensitive, or distorted form. Cortical remapping is required to refine this raw, mismatched peripheral signal back into usable, accurate touch awareness, proving that regrowth alone does not guarantee full function.
What specific treatments maximize the chance that full sensory function returns after nerve damage?
The treatments most likely to maximize the chance that full sensory function returns after nerve damage are those that improve reinnervation quality, support the repair environment metabolically, and help the nervous system refine the returning signal rather than simply waiting for any regrowth to occur.
Addressing the factors that slow dermal nerve recovery means acknowledging that biological nerve regeneration is a two-part problem: fueling the physical wire, and retraining the brain to understand it.
How does sensory re-education maximize the chance that full sensory function returns after nerve damage?
Sensory re-education maximizes the chance that full sensory function returns after nerve damage by helping the brain relearn texture, pressure, and location cues once some signal has begun to return, especially when the early returning sensation is distorted or hypersensitive.
Controlled texture tracing, temperature mapping, and structured touch training actively force the brain to refine the cortical interpretation of scrambled inputs.
This rehabilitation stage becomes exceptionally critical once baseline sensory return exists, converting messy raw regrowth into refined functional sensibility.
How do B-vitamins and metabolic support maximize the chance that full sensory function returns after nerve damage?
B-vitamins and broader metabolic support may maximize the chance that full sensory function returns after nerve damage by improving the biochemical environment for peripheral nerve maintenance and repair, but they should be presented as supportive measures rather than guarantees of complete recovery.
Vitamin B12 is thoroughly documented as essential for myelin sheath repair and rigorous neuronal metabolism, providing the necessary energetic foundation for the growth cone.
While establishing this robust metabolic environment is critical for preventing stalled growth, metabolic support alone cannot physically force an axon to connect to the correct topographic target if the guidance architecture is destroyed.
Sensory Recovery Optimization Pathway
- Problem → nerve regrows but function remains incomplete or poorly refined.
- Implication → sensation may stay numb, hypersensitive, or mismatched.
- Solution → improve reconnection conditions, support metabolism, and retrain the sensory system.
What are the key summary facts regarding whether full sensory function returns after nerve damage?
The key summary facts are that full sensory function can return after nerve damage, but it depends on accurate reconnection rather than regrowth alone, and the final outcome is shaped by injury type, guidance quality, regrowth distance, tissue health, and sensory re-education.
Summary Checklist
What steps can you take to help ensure full sensory function returns after nerve damage today?
The chance that full sensory function returns after nerve damage improves when patients protect the repair environment, support metabolic health, use sensory re-education appropriately, and seek specialist review when recovery becomes distorted or stalls.
Final Execution Checklist
Quick Answers About Whether Full Sensory Function Returns After Nerve Damage
Can full sensory function return after nerve damage?
Full sensory function can return after nerve damage, but it requires precise biological regrowth and accurate target reinnervation. The probability of complete sensory return after nerve damage depends heavily on injury severity.
What does full sensory recovery actually require?
Full sensory recovery requires structural continuity, accurate target matching, and brain-level interpretation. If the axon reconnects but targets the wrong sensory receptor, full sensory function returns after nerve damage in a distorted or mismatched form.
Do mild nerve injuries recover more completely than severe ones?
Yes. Mild injuries like neurapraxia preserve the internal guidance structures, ensuring a high probability of recovery. Severe transection injuries scramble these pathways, severely lowering the chance that full sensory function returns after nerve damage.
Why can skin heal before sensation returns?
Skin closes rapidly through epidermal cell division, while peripheral nerve regeneration proceeds slowly at approximately 1 millimeter per day. This biological speed limit creates delayed sensory return after skin healing is visibly complete.
What is topographic precision in nerve recovery?
Topographic precision refers to the exact, correct reconnection of a regrowing nerve fiber to its original tissue target. Without this strict alignment, sensory return after peripheral nerve injury feels vague, scrambled, or hypersensitive.
How do Schwann cells help sensory return?
Repair Schwann cells form physical guidance tunnels and secrete chemical signals that direct the advancing growth cone. Because Schwann cells guide sensory reconnection, they prevent the regenerating nerve from wandering aimlessly into surrounding scar tissue.
Can sensory re-education improve recovery quality?
Yes. Sensory re-education improves functional recovery by using targeted physical stimuli to induce cortical remapping. This helps the brain correctly interpret returning, often distorted signals, proving that regrowth does not guarantee full function alone.
Do age and diabetes lower the odds of complete return?
Yes. Age and poor metabolic health impair microvascular blood flow and cellular repair efficiency. Because these factors damage the healing environment, full sensory function returns after nerve damage less reliably in diabetic or older patients.
Conclusion
In conclusion, full sensory function can return after nerve damage only when biological regrowth, pathway precision, and sensory reinterpretation all work together, which is why complete recovery remains possible but never automatic.
By understanding that regenerating a nerve involves reconnecting millions of delicate biological wires across a vast distance to exact microscopic targets, the timeline of healing becomes far more logical. Supporting this repair environment through metabolic health, minimizing scar obstruction, and utilizing sensory re-education transforms raw cellular regrowth into clear, accurate touch awareness over time.