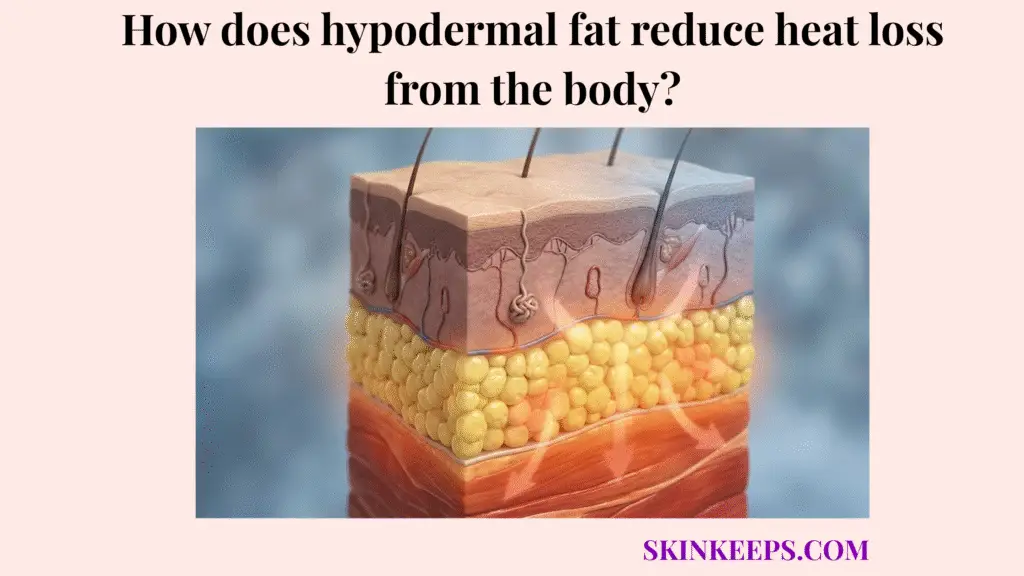
Hypodermal fat reduces heat loss from the body by forming an insulating layer beneath the skin that slows heat transfer from warmer internal tissues to the cooler external environment.
Hypodermal fat is the main subcutaneous insulating layer and does not work alone. Skin blood flow control, fat thickness, and fat distribution all affect how much heat loss can be prevented.
This article will explain why this matters, when it matters most, how the insulation begins beneath the skin, how it works with blood flow, how low and high fat levels change protection, and when insulation is not enough on its own.
Why Hypodermal Fat Reduction of Body Heat Loss Matters
Hypodermal fat reduction of body heat loss matters because it helps preserve core warmth by limiting unnecessary outward heat escape.
The main value of hypodermal fat in this context is not energy storage, but heat conservation. Core warmth is a strict biological requirement, and protecting it means blocking the fast exit of thermal energy.
Internal temperature depends not only on heat production, but also on how quickly heat leaves the body. Passive insulation acts as the first line of defense before the body has to burn calories to stay warm.
The next sections will explain when this protection matters most and how the mechanism works anatomically and physiologically.
| Function | How hypodermal fat performs it | Effect on body heat loss reduction |
|---|---|---|
| Insulation | Resists heat transfer | Helps conserve body heat |
| Heat transfer slowing | Creates subcutaneous resistance | Protects core temperature |
| Heat loss reduction | Lowers passive heat escape | Better cold tolerance |
| Thermal buffering | Slows sudden temperature shifts | More stable internal temperature |
Why Hypodermal Fat Helps Preserve Core Warmth
Hypodermal fat helps preserve core warmth because it slows the outward movement of heat from deeper tissues toward the skin surface.
Core warmth is protected when less heat escapes from deeper tissues into the surrounding environment. The physical barrier simply makes it harder for that heat to leave.
This does not mean the body generates extra heat here; it means the body loses existing heat more slowly. The insulation traps what is already there.
Preserved core warmth directly links to better tolerance of cold or cooling environments, giving the body an immediate survival advantage.
Why Hypodermal Fat Helps the Body Resist Unnecessary Heat Escape
Hypodermal fat helps the body resist unnecessary heat escape because it forms a passive thermal barrier between the warm body interior and the cooler outside environment.
“Unnecessary heat escape” means passive loss of heat that the body would rather conserve. It is an unwanted leak that forces the body to work harder to stay warm.
While there is ongoing research into whether brown fat can generate heat within the hypodermis, typical white subcutaneous fat reduces this passive outward movement without requiring active thermoregulatory effort like shivering. It provides continuous, free defense.
This makes insulation especially valuable before stronger active defenses are required, acting as a buffer that saves metabolic energy.
When Hypodermal Fat Reduction of Body Heat Loss Occurs Most Strongly
Hypodermal fat reduction of body heat loss occurs most strongly when environmental conditions favor rapid outward heat escape, especially during cold exposure.
The effect is strongest when the environment is colder than the body and therefore pulls heat outward more aggressively. Heat naturally flows toward cold, and a stronger gradient demands stronger resistance.
The importance of insulation rises as the risk of passive heat loss rises. When the body is not under thermal threat, this insulation operates quietly in the background.
Both cold exposure and general heat-loss conditions amplify the value of subcutaneous insulation, shifting it from a background feature to a vital survival tool.
When Cold Exposure Increases Hypodermal Fat Reduction of Body Heat Loss
Cold exposure increases hypodermal fat reduction of body heat loss when the temperature difference between the body and the environment becomes large enough to accelerate outward heat movement.
Colder external conditions create a stronger pull for heat to leave the body. The thermal gradient essentially tries to drain the body of its warmth.
The same amount of insulation matters more under stronger cold stress. The tissue does not change, but its protective value skyrockets relative to the threat.
This is why hypodermal fat becomes most obviously protective during cold exposure rather than in thermally neutral conditions where heat loss is already minimal.
When Environmental Heat Loss Makes Subcutaneous Insulation More Important
Environmental heat loss makes subcutaneous insulation more important whenever the surroundings favor rapid transfer of heat away from the skin.
Air, water, and wind can all increase heat loss from the body surface. A cold wind strips away the warm boundary layer of air around the skin instantly.
When surface heat is lost faster, insulation beneath the skin becomes more important in slowing continued heat escape from deeper tissues. It is the final wall holding the core temperature stable.
Environmental conditions directly shape the value of subcutaneous fat in heat conservation, proving that insulation is highly context-dependent.
How Hypodermal Fat Reduction of Body Heat Loss Begins Beneath the Skin
Hypodermal fat reduction of body heat loss begins beneath the skin because the hypodermis forms the body’s main subcutaneous insulating layer.
The hypodermis is positioned deep in the body wall, constructed primarily of adipose and connective tissues. This gives it the bulk necessary to act as a physical barrier.
It is positioned between deeper tissues and the external environment, which gives it prime thermal relevance. It is the gatekeeper for heat exiting the core.
Both the structure and the position of the hypodermis matter heavily for heat-loss reduction, as location determines what it can protect.
How Hypodermal Fat Forms the Body’s Main Subcutaneous Insulating Layer
Hypodermal fat forms the body’s main subcutaneous insulating layer because the hypodermis contains adipose tissue that resists heat transfer more than more vascular tissues.
The hypodermis is adipose-rich, and adipose tissue forms the physical thermal basis of insulation here. Fat is uniquely suited to block energy transfer.
This makes the hypodermis the main insulating layer beneath the skin rather than the dermis itself, which is heavily vascularized and prone to heat exchange.
Tissue composition connects directly to heat-loss reduction, proving that anatomy drives thermal function.
How Hypodermal Fat Sits Between Deeper Tissues and the Cooler Outside Environment
Hypodermal fat sits between deeper tissues and the cooler outside environment, which places it directly in the path of outward heat transfer.
The hypodermis sits securely beneath the dermis and above deeper muscular structures. It acts as an anatomical sandwich layer wrapping the entire body.
This location intercepts outward heat movement before that heat reaches the environment. It catches the thermal energy while it is still safely inside.
The hypodermis is anatomically placed perfectly to act as a subcutaneous heat-loss barrier, halting the progression of cooling.
How Hypodermal Fat Reduction of Body Heat Loss Works by Slowing Heat Transfer
Hypodermal fat reduction of body heat loss works by slowing heat transfer because adipose tissue has low thermal conductivity.
The physical mechanism relies on the fact that hypodermal fat conducts heat poorly. It naturally resists the fast transmission of thermal energy through its cellular structure.
Practically, heat from warmer internal tissue does not pass outward as quickly through this barrier. The heat is forced to stall.
Both low conductivity and slower heat movement are central to the preservation mechanism, converting anatomical padding into a physiological shield.
How Low Thermal Conductivity Supports Hypodermal Fat Reduction of Body Heat Loss
Low thermal conductivity supports hypodermal fat reduction of body heat loss by making adipose tissue resist heat movement better than many other tissues.
Low thermal conductivity simply means that heat does not pass through adipose tissue efficiently. The molecular makeup of fat blocks easy energy exchange.
Poor conduction effectively slows the transfer of warmth toward the superficial skin boundary, keeping it locked inside the body longer.
This is the core physical reason hypodermal fat works as an insulator; subcutaneous fat thermal conductivity has been measured at about 0.23 W/m·K (El-Brawany, 2009).
How Slower Heat Movement Protects Deeper Body Warmth
Slower heat movement protects deeper body warmth by reducing the speed at which internal heat travels from the core toward the surface.
Slower heat movement means the body’s internal warmth is depleted much more gradually, avoiding sudden, dangerous drops in temperature.
This is especially important for preserving vital warmth in deeper tissues and the core, where organs must remain at a stable temperature to function.
Slower heat movement is directly tied to highly effective heat-loss reduction, buying the body time to react.
How Hypodermal Fat Reduction of Body Heat Loss Works at the Skin Boundary
Hypodermal fat reduction of body heat loss works at the skin boundary by limiting how much internal heat reaches the surface and becomes available to escape into the environment.
Body heat must reach the skin surface before it can be lost outward via radiation, convection, conduction, or evaporation. The surface is the only exit door.
Subcutaneous insulation forcefully reduces the supply of heat reaching that boundary. It cuts off the thermal supply line.
This fundamentally weakens the overall chain of heat escape from the body interior to the environment, trapping the heat safely below the skin.
How Hypodermal Fat Reduction of Body Heat Loss Works With Blood Flow Control
Hypodermal fat reduction of body heat loss works with blood flow control because blood flow determines how much heat reaches the skin, while fat determines how efficiently that heat can continue outward.
Insulation and blood flow must be understood together, not as separate systems. Understanding what role blood flow plays in hypodermal heat retention clarifies how they act as a coordinated thermal defense mechanism.
Skin blood flow is the main controllable path for moving core heat toward the environment. When the vessels open, heat rushes past the fat layer.
Reduced blood flow strengthens insulation, while full heat-loss control still depends on more than fat alone.
How Reduced Skin Blood Flow Strengthens Hypodermal Fat Reduction of Body Heat Loss
Reduced skin blood flow strengthens hypodermal fat reduction of body heat loss because less warm blood reaches the skin surface, so less heat is available to escape.
Less warm blood at the skin means less heat is available near the surface. The body actively starves the outer perimeter of thermal energy.
This makes passive subcutaneous insulation drastically more efficient, as it now guards a lower volume of heat.
Vasoconstriction and insulation perfectly reinforce one another during cold protection, acting as a dual-layer defense system.
How Hypodermal Fat Reduction of Body Heat Loss Depends on More Than Insulation Alone
Hypodermal fat reduction of body heat loss depends on more than insulation alone because the body also relies on circulation, central thermoregulation, and active heat-conserving responses.
Hypodermal fat is only one part of the thermoregulatory system. It is a passive barrier that cannot adapt in real-time.
The hypothalamus, vasoconstriction, shivering, and behavioral changes all help limit heat loss too, actively adjusting to environmental threats.
Fat insulation is strongest when it works inside a larger coordinated heat-conservation system, providing the base resistance the active systems need to succeed.
Why Hypodermal Fat Reduction of Body Heat Loss Protects Against Rapid Cooling
Hypodermal fat reduction of body heat loss protects against rapid cooling because subcutaneous insulation slows the rate of temperature change rather than only reducing total heat loss.
Rapid cooling is a rate problem as much as it is a total heat-loss problem. An abrupt drop in temperature can shock the system before it can react.
Subcutaneous fat functions as a thermal buffer by slowing how fast warmth is lost, effectively buying time.
Slower cooling directly provides better thermal stability and more physiological response time, allowing shivering and vasoconstriction to deploy safely.
How Low Hypodermal Fat Weakens Body Heat Loss Reduction
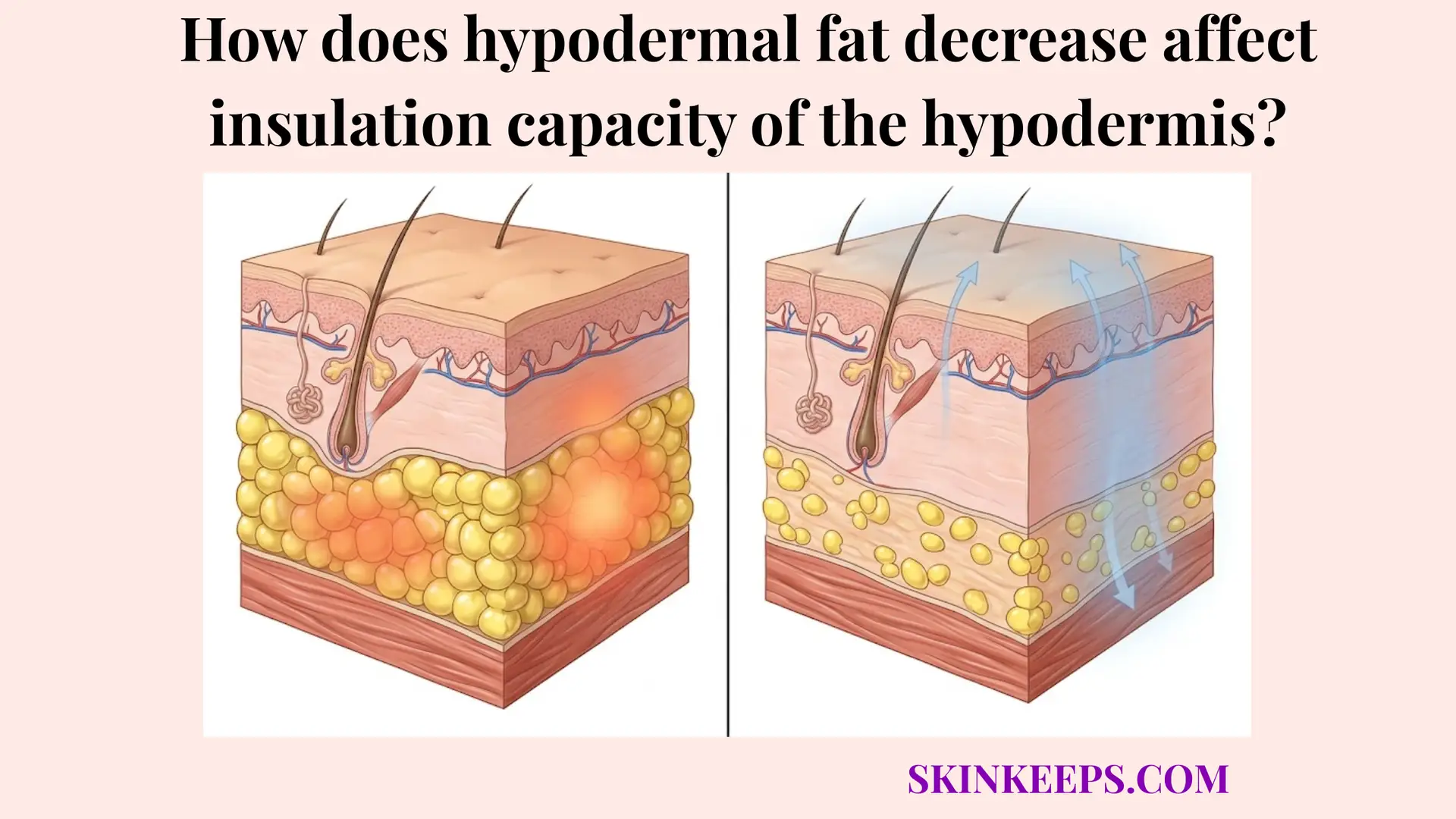
Low hypodermal fat weakens body heat loss reduction because thinner subcutaneous insulation offers less resistance to outward heat movement.
Low subcutaneous fat means less physical insulation beneath the skin. The barrier is mechanically deficient. Assessing how does hypodermal fat decrease affect insulation capacity of the hypodermis? reveals that weaker insulation allows internal heat to escape much more easily.
Weaker insulation allows internal heat to escape more easily, as the distance to the cold environment is drastically shortened.
This raises heat-loss vulnerability and directly weakens cold protection, forcing the body to rely entirely on burning calories to stay warm.
How Low Hypodermal Fat Increases Outward Heat Escape
Low hypodermal fat increases outward heat escape because less insulating tissue means less resistance to heat transfer from deeper tissues to the surface.
Outward heat escape rises aggressively when the subcutaneous barrier becomes thinner. The insulation is structurally compromised.
This affects passive heat loss even before stronger cold-defense responses begin to work, causing a constant, low-level energy drain.
Reduced insulation weakens basic heat-conservation capacity at a fundamental anatomical level.
How Reduced Insulation Makes the Body More Vulnerable to Cold Loss
Reduced insulation makes the body more vulnerable to cold loss because heat can leave the body faster in cold conditions when subcutaneous protection is limited.
Cold environments expose the weakness of low insulation more clearly than neutral environments do, turning a minor chill into a deep freeze.
People with low subcutaneous fat may feel cold sooner and depend more heavily on active defenses like shivering to generate replacement heat.
Reduced insulation lowers thermal resilience in cold conditions significantly, marking a clear physiological disadvantage in winter climates.
How Excess Hypodermal Fat Changes Body Heat Loss Reduction
Excess hypodermal fat changes body heat loss reduction by strengthening insulation and reducing passive heat escape, while also creating tradeoffs when the body needs to release heat.
Stronger subcutaneous insulation can effectively reduce body heat loss and preserve warmth, creating excellent cold tolerance.
However, stronger insulation is not always better across all environments; thermal defense requires balance.
Higher fat can help cold protection while also complicating heat release in other conditions, turning a winter advantage into a summer liability.
| Fat level | Insulation strength | Passive heat escape | Cold protection | Heat release efficiency |
|---|---|---|---|---|
| Low fat | Weak | Rapid | Lower tolerance | High efficiency |
| Moderate fat | Balanced | Controlled | Standard | Manageable |
| Higher fat | Strong | Severely reduced | High tolerance | Can be inefficient or impaired |
How Thicker Hypodermal Fat Can Improve Body Heat Loss Reduction
Thicker hypodermal fat can improve body heat loss reduction by increasing the depth and resistance of the subcutaneous insulating layer.
Greater subcutaneous thickness increases the physical distance heat must cross to escape. It provides more padding against the cold.
This can greatly improve body heat retention, especially in freezing or cold settings where passive loss is a threat.
Higher insulation can absolutely strengthen cold protection when heat conservation is the main goal.
How Excess Insulation Can Complicate Heat Release in Other Conditions
Excess insulation can complicate heat release in other conditions because the same tissue that helps conserve heat in the cold can slow heat dissipation in heat stress.
Heat-conservation advantages quickly become biological disadvantages when the body needs to unload heat quickly to avoid overheating.
This is especially relevant in hot environments or during intense exercise heat stress, where the core temperature threatens to spike dangerously.
Higher subcutaneous insulation improves one side of thermoregulation while complicating the other. Speakman and Westerterp (2018) noted that obesity can provide an advantage in cold conditions but can also make people more susceptible to heat stress than lean individuals [PubMed].
Which Factors Affect Hypodermal Fat Reduction of Body Heat Loss
Several factors affect hypodermal fat reduction of body heat loss, especially fat thickness, body composition, age, metabolism, fat distribution, environment, clothing, and activity level.
Body-level factors such as fat thickness and body composition dictate baseline insulation strength.
Physiologic and demographic factors such as age, metabolism, and fat distribution further modify efficiency and resilience.
External and behavioral factors such as environment, clothing, and activity level influence ultimate effectiveness in the real world.
Which Roles Fat Thickness and Body Composition Play in Body Heat Loss Reduction
Fat thickness and body composition affect body heat loss reduction by changing how much insulating tissue lies beneath the skin and how much lean tissue remains available for heat transfer.
Thicker subcutaneous fat usually improves overall insulation, physically blocking energy loss.
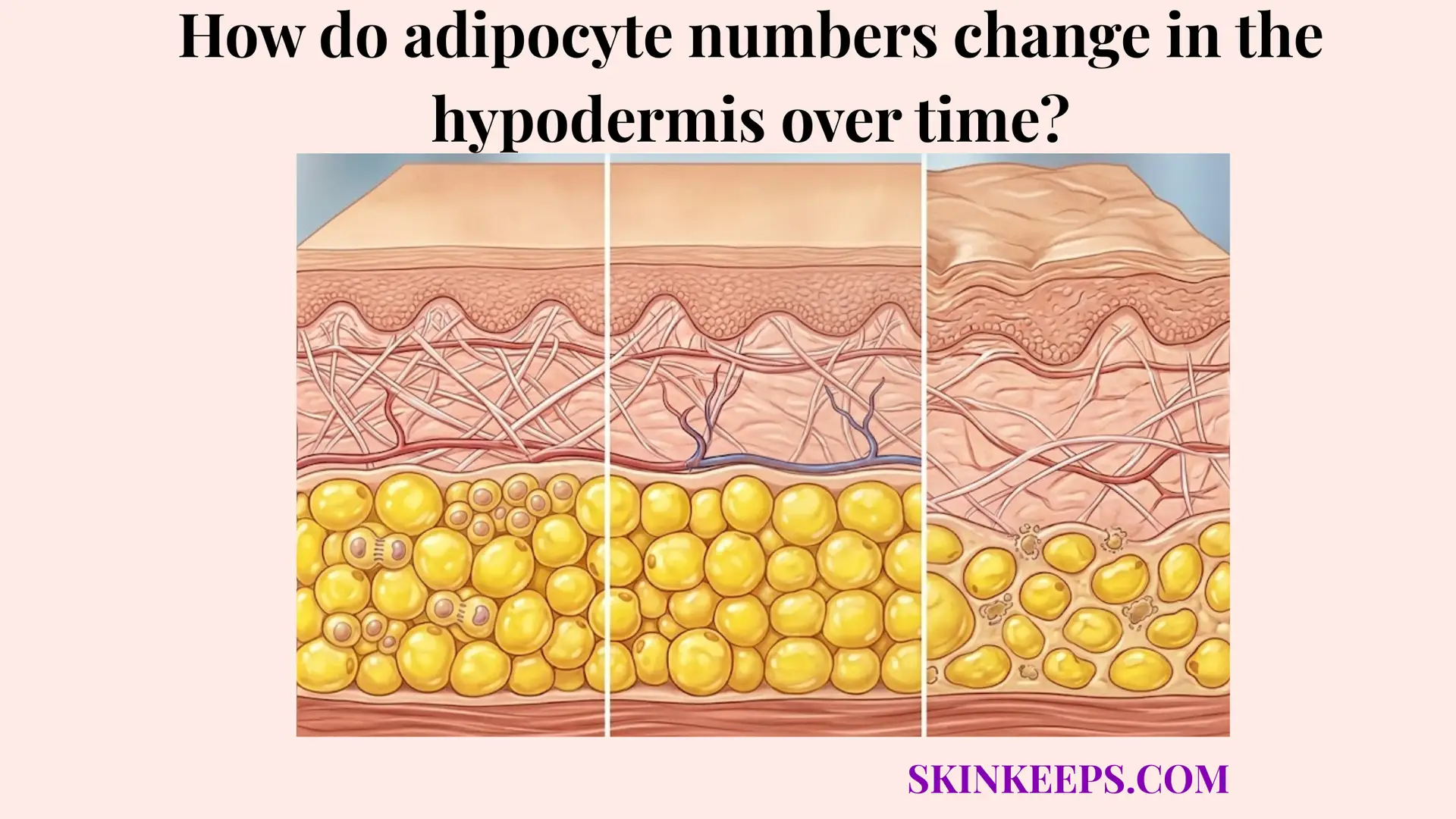
Body composition directly influences the structural strength of passive heat-loss protection. Recognizing how do adipocyte numbers change in the hypodermis over time? is critical for evaluating long-term thermal resilience.
Body composition directly influences the structural strength of passive heat-loss protection.
Which Roles Age, Metabolism, and Fat Distribution Play in Body Heat Loss Reduction
Age, metabolism, and fat distribution affect body heat loss reduction because insulation strength depends not only on fat amount, but also on where fat is stored and how the body responds to cold.
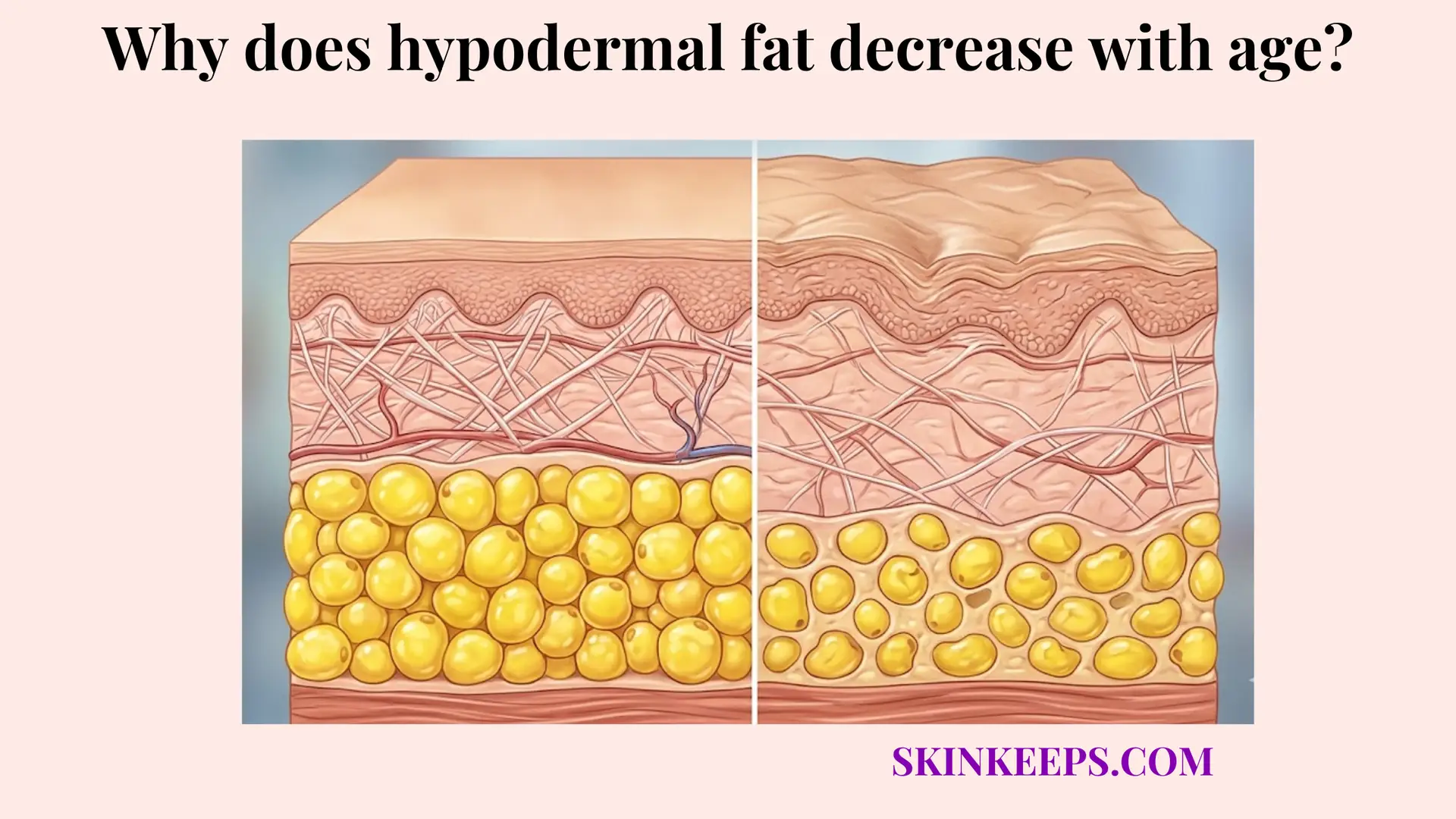
Age can alter both subcutaneous insulation volume and broader thermoregulatory vascular capacity, making older adults more vulnerable. Exploring why does hypodermal fat decrease with age? helps explain this progressive loss of thermal defense.
Metabolism matters deeply because heat conservation works differently when internal heat production changes due to thyroid or cellular health.
Regional fat pattern matters just as much as total adiposity when determining protection against localized cooling.
Which Roles Environment, Clothing, and Activity Level Play in Body Heat Loss Reduction
Environment, clothing, and activity level affect body heat loss reduction because they change both the demand for insulation and the body’s need to either conserve or release heat.
Colder, wetter, or windier conditions drastically increase the importance of physical insulation, pushing the body to its limits.
Clothing adds necessary external insulation and can strongly reinforce the protective effect of subcutaneous fat by trapping a layer of warm air.
Activity changes internal heat production, which dictates whether conserving heat is useful or severely limiting to athletic performance.
How Hypodermal Fat Reduction of Body Heat Loss Compares With Other Protective Mechanisms
Hypodermal fat reduction of body heat loss differs from other protective mechanisms because it is mainly a passive insulating process, while vasoconstriction, shivering, and metabolic heat production are active responses.
Hypodermal fat acts exclusively as passive insulation, not as an active thermoeffector that turns on and off.
Active mechanisms generate heat or actively shunt blood to conserve it based on immediate brain signals.
The strongest heat-loss protection happens when passive insulation and active responses work together flawlessly.
How Hypodermal Fat Reduction of Body Heat Loss Compares With Vasoconstriction
Hypodermal fat reduction of body heat loss compares with vasoconstriction in that fat slows passive heat transfer, while vasoconstriction reduces the delivery of warm blood to the skin surface.
Hypodermal insulation provides constant physical resistance to heat movement, acting as a permanent wall.
Vasoconstriction circulatorily starves the surface of warm blood to keep heat deep inside, acting as an adjustable valve.
Both reduce heat loss, but through entirely different mechanical routes.
How Hypodermal Fat Reduction of Body Heat Loss Compares With Shivering and Metabolic Heat Production
Hypodermal fat reduction of body heat loss compares with shivering and metabolic heat production in that insulation conserves existing heat, while shivering and metabolism increase heat generation.
Hypodermal fat helps keep existing heat inside the body, preserving what is already there.
Shivering and metabolism help create or sustain new heat from within, burning calories to replace what was lost.
Conservation and production are complementary, essential parts of total cold protection.
How Regional Fat Distribution Changes Body Heat Loss Reduction
Regional fat distribution changes body heat loss reduction because insulation is not uniform across the body, and some areas have much less subcutaneous protection than others.
Body fat is not spread evenly, and local insulation differs dramatically by region, altering thermal defense mapping.
Some body areas therefore lose heat substantially faster than others when exposed to the same cold air.
Regional distribution changes local heat-loss reduction even if total body fat is similar between two individuals.
How Body Areas With Less Hypodermal Fat Lose Heat Faster
Body areas with less hypodermal fat lose heat faster because thinner subcutaneous insulation provides less resistance to outward heat transfer.
Local heat loss depends heavily on local subcutaneous thickness, making the anatomy the dictating factor.
Thinner areas allow faster outward heat movement and rapid cooling, which is why fingers and ears freeze quickly.
Body heat-loss reduction is simply not equally strong everywhere on the body.
How Uneven Subcutaneous Insulation Changes Local Body Heat Loss Reduction
Uneven subcutaneous insulation changes local body heat loss reduction by making some regions better protected than others against outward heat escape.
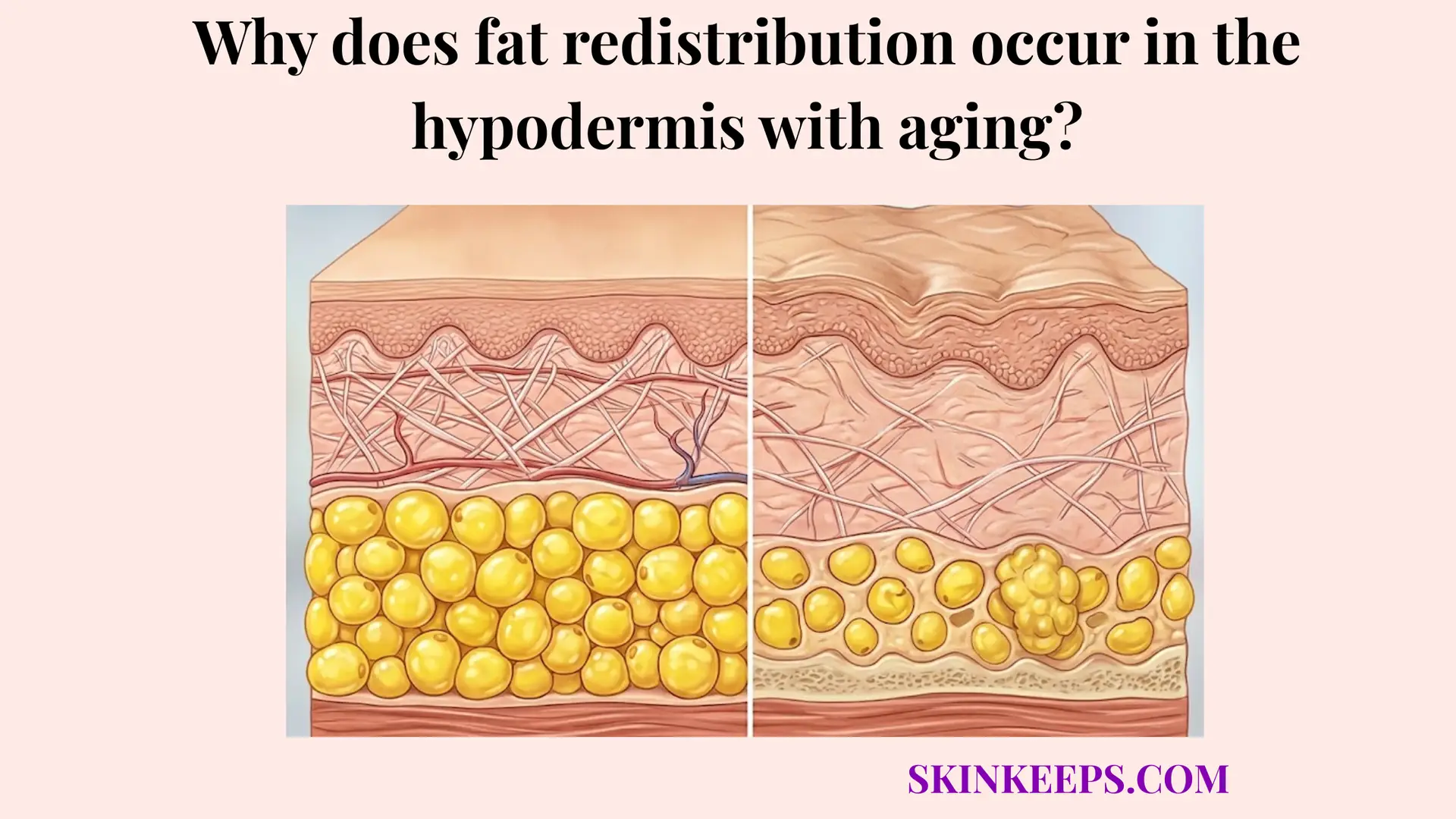
Not all body regions have the same insulating architectural depth, causing thermal imbalances. Learning why does fat redistribution occur in the hypodermis with aging? shows how these local vulnerabilities can shift across different life stages.
This uneven structure creates distinct regional differences in heat-loss tendency.
Local insulation variation is directly linked to regional cooling patterns. Savastano et al. (2009) noted that regional subcutaneous adipose tissue provides an insulating layer that impedes heat loss and may blunt abdominal heat transfer [PMC].
When Hypodermal Fat Reduction of Body Heat Loss Is Not Enough on Its Own
Hypodermal fat reduction of body heat loss is not enough on its own when external cold overwhelms passive insulation or when broader thermoregulatory support is insufficient.
Insulation alone cannot guarantee adequate heat conservation under all extreme conditions; it has a biological breaking point.
Extreme cold, weak circulation, low metabolic response, or insufficient clothing can quickly overwhelm passive protection and threaten core temperature.
Both environmental severity and physiologic limitation determine exactly when extra protection is needed to survive.
When External Cold Overwhelms Hypodermal Fat Reduction of Body Heat Loss
External cold overwhelms hypodermal fat reduction of body heat loss when the environment pulls heat outward faster than passive subcutaneous insulation can resist.
Stronger cold exposure means a much stronger gradient for heat loss, ripping warmth away from the skin surface.
Beyond a certain point, passive insulation is mathematically not enough by itself to stop the drain.
Stronger active defenses and external physical protection then become absolutely necessary to avoid hypothermia.
When Extra Protection Is Needed Beyond Subcutaneous Insulation
Extra protection is needed beyond subcutaneous insulation when body heat conservation requires help from clothing, shelter, behavior change, or stronger physiologic responses.
Clothing and shelter are major external tools required when body heat loss risk rises aggressively in extreme weather.
Behavior and active cold defenses matter exponentially more when passive insulation is limited by low body fat.
Hypodermal fat is important, but it is not sufficient in every cold challenge, requiring humans to rely on adaptation.
Which Key Takeaways Define Hypodermal Fat Reduction of Body Heat Loss
The key takeaways are that hypodermal fat reduces body heat loss by forming the main subcutaneous insulating layer, slowing heat transfer, reducing outward heat escape, and helping preserve core warmth.
Hypodermal fat reduces body heat loss by slowing heat transfer physically through its poor conductivity.
Blood flow, vasoconstriction, and other active responses still matter intensely for overall thermal balance.
Low fat weakens protection, while higher fat can improve insulation but complicate heat release elsewhere, confirming the central biological tradeoff.
What to Remember About Hypodermal Fat Reduction of Body Heat Loss
Quick Answers About Hypodermal Fat Reduction of Body Heat Loss
Does hypodermal fat keep the body warm or just reduce heat loss?
Hypodermal fat reduces heat loss rather than keeping the body warm by itself. It functions as a passive physical barrier that slows the outward movement of heat already generated by deep metabolic tissues.
Why does subcutaneous fat matter more in the cold?
Subcutaneous fat matters more in the cold because freezing environments create a massive temperature gradient that forcefully pulls heat outward. A thick layer of insulation is required to resist that aggressive physical demand.
Does low body fat make people lose heat faster?
Yes. Low body fat drastically reduces the thickness of the subcutaneous insulating layer, presenting less physical resistance to outward heat transfer and resulting in significantly faster passive heat loss.
Can more fat improve cold protection?
Yes. A thicker layer of hypodermal fat actively improves cold protection by extending the physical distance heat must cross to escape, fundamentally reducing passive heat loss and improving cold tolerance.
Can more fat make heat harder to release?
Yes. The same robust insulation that excellently slows heat loss in the cold acts as a strict biological limitation during severe heat stress, severely hindering the body’s ability to dissipate dangerous internal warmth.
How does blood flow affect heat loss even when fat insulation is present?
Skin blood flow actively bypasses insulation by carrying warm blood close to the surface for release (vasodilation) or trapping it deep within the core (vasoconstriction), completely dictating real heat loss dynamics.
Why is clothing still important if subcutaneous fat already insulates?
Subcutaneous fat insulation possesses strict biological limits. In severe cold or intense wind, external barriers like clothing are absolutely necessary because passive internal insulation alone cannot halt massive outward heat transfer.
Is body heat-loss protection the same in all body regions?
No. Body heat-loss protection is regionally uneven because subcutaneous fat thickness varies. Body parts with less padding provide less resistance to outward heat flow and invariably cool much faster.
Conclusion
Hypodermal fat reduces heat loss from the body by forming an insulating layer beneath the skin that slows heat transfer from warmer internal tissues to the cooler external environment.
Insulation beneath the skin slows outward heat transfer and reliably reduces passive heat loss, serving as the biological foundation of cold defense.
Blood flow control, vasoconstriction, shivering, and external protection all work with insulation rather than being replaced by it, orchestrating a complex, full-body thermal response.
Hypodermal fat ultimately stands as the body’s main subcutaneous heat-loss barrier, proving itself exceptionally valuable during cold exposure and serving as a crucial component of human survival.