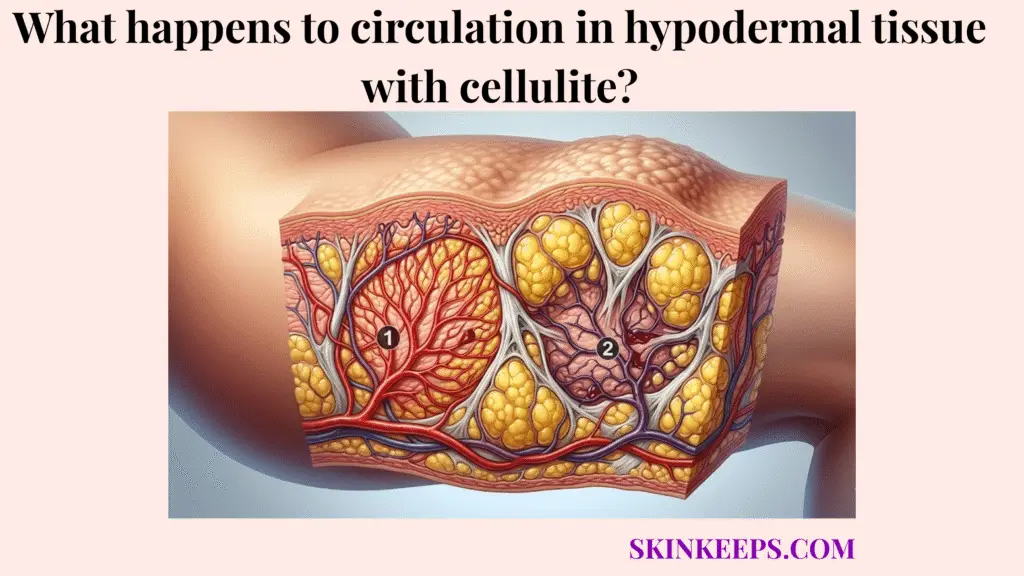
Circulation in cellulite-affected hypodermal tissue may become less efficient when enlarged fat lobules, fibrous septae, and fluid pressure interfere with microvascular flow and lymphatic drainage. These structural restrictions disrupt normal angiologic tissue flow, leading to localized fluid imbalance and altered oxygenation.
This physiological guide explains how blood flow and lymphatic drainage respond to these architectural changes within the subcutaneous layer. It clarifies the realities of tissue hypoxia, debunks common lifestyle triggers and detox myths, and outlines realistic expectations for daily management and clinical intervention.
What is the normal biological function of microvascular flow in healthy subcutaneous fat?
The normal biological function of microvascular flow in healthy subcutaneous fat is to deliver oxygen and nutrients through small vessels while lymphatic drainage removes excess interstitial fluid from the tissue environment. The hypodermis supports adipose storage, insulation, and structural anchoring by relying on this steady circulatory exchange.
When this baseline perfusion operates correctly, the soft tissue remains well-oxygenated and mechanically stable. Any interruption to this delicate plumbing system naturally creates functional imbalances within the fat layer.
How do capillaries and lymphatic vessels support hypodermal tissue?
Capillaries and lymphatic vessels support hypodermal tissue by maintaining oxygen delivery, nutrient exchange, and fluid return within the subcutaneous fat layer. This capillary network supplies the vital oxygen required for healthy adipocyte function.
Simultaneously, the lymphatic vessels gently sweep away excess water and proteins to prevent localized tissue swelling. Cellulite is present in approximately 80–90% of postpubertal women, which makes circulation and fluid balance in cellulite-prone hypodermal tissue clinically relevant to many readers. [PubMed]
How does interstitial fluid balance keep subcutaneous tissue stable?
Interstitial fluid balance keeps subcutaneous tissue stable by preventing excess fluid from accumulating between adipocytes, fibrous septae, and small vessels. This interstitial fluid acts as the watery medium surrounding all local tissue cells.
When blood vessels and lymphatic channels move this fluid efficiently, the tissue avoids unnecessary swelling and pressure. Maintaining this balance ensures the structural architecture remains firm rather than waterlogged.
Why do enlarged adipocytes reduce local hypodermal blood supply?
Enlarged adipocytes can reduce local hypodermal blood supply by increasing tissue pressure inside fat compartments and narrowing the space available for small vessels and lymphatic channels. Because fat protrusion alters hypodermal surface structure, this same physical expansion simultaneously crowds the delicate internal plumbing.
As fat cells expand within rigid septal walls, the enclosed compartment simply runs out of room. This internal compression forces the soft, pliable capillary walls to narrow.
How does the vascular compression effect restrict microcirculation?
The vascular compression effect restricts microcirculation when enlarged fat lobules and stiff connective compartments increase pressure around small vessels. These fragile micro-vessels lack the muscular walls of larger arteries, making them highly susceptible to external squeezing.
When surrounding fat lobules compress them, local blood flow inevitably becomes less efficient. This restricted perfusion slightly diminishes the overall oxygen and nutrient delivery to the affected tissue.
How do lymphatic compression and edema interact?
Lymphatic compression and edema interact because low-pressure lymphatic vessels may drain fluid less efficiently when surrounding tissue pressure rises. Lymphatic channels are remarkably thin and easily compressed by expanding fat compartments.
When their drainage capacity drops, excess fluid remains trapped in the interstitial spaces, leading to localized edema. This subtle fluid retention makes tissue swelling and surface texture prominence visibly worse.
| Tissue State | Blood Flow Pattern | Lymphatic Drainage | Interstitial Fluid Level |
|---|---|---|---|
| Healthy subcutaneous fat | Efficient capillary perfusion | Fluid returns through lymphatics | Stable fluid environment |
| Enlarged adipocyte compartments | Small-vessel space may narrow | Drainage may become less efficient | Fluid may accumulate |
| Cellulite-prone tissue | Microcirculation may be less efficient | Fluid movement may slow | Texture may look more swollen |
| Sedentary lower body | Muscle-pump activity decreases | Fluid return may slow | Dependent pooling may increase |
| Restrictive clothing zones | Local pressure increases | Flow may be mechanically limited | Temporary swelling or indentation may appear |
How does prolonged tissue hypoxia accelerate hardening of fibrotic cellulite bands?
Prolonged tissue hypoxia may accelerate hardening of fibrotic cellulite bands by promoting inflammatory signaling, fibroblast activation, and increased collagen deposition within the hypodermal support network. When microcirculation slows, the tissue experiences this subtle reduction in oxygen availability.
This low-grade fibrous septa create hypodermal skin dimpling environment reacts by thickening the connective tissue. Ultimately, this structural hardening cements the tethering effect.
How does the hypoxia-inflammation cycle affect cellulite tissue?
The hypoxia-inflammation cycle affects cellulite tissue when reduced oxygen availability supports inflammatory signaling that can make the local connective environment stiffer. This subtle ischemia-like stress triggers local cells to release signaling cytokines.
These cytokines may stimulate a low-grade inflammatory response within the fat compartment. Over time, this mild but persistent inflammation supports ongoing tissue rigidity.
How do fibroblast activation and sclerosis deepen dimpling?
Fibroblast activation and sclerosis may deepen dimpling when connective tissue cells produce denser collagen that stiffens the septal network around fat lobules. Fibroblasts act as the primary collagen-producing cells within the dermis and hypodermis.
When activated by inflammatory signals, they deposit thicker, less elastic collagen fibers, leading to tissue sclerosis. This targeted stiffening increases the downward pull on the skin surface, visibly deepening the localized dimples.
Which mechanical lifestyle habits worsen lymphatic fluid stagnation in the lower body?
Mechanical lifestyle habits can worsen lymphatic fluid stagnation in the lower body when they reduce muscle-pump activity, increase local pressure, or limit comfortable movement through the hips, thighs, and legs. Our vascular system relies heavily on physical movement to defy gravity and return fluids upward.
When lifestyle choices impede this mechanical assistance, fluid naturally pools in dependent tissues. Recognizing these habits is the first step toward practical fluid management.
How does prolonged sedentary behavior reduce fluid return?
Prolonged sedentary behavior can reduce fluid return because leg muscles contract less often, limiting the pumping action that helps move venous blood and lymphatic fluid out of the lower body. The calf muscle pump actively squeezes deep veins during walking to propel fluids upward.
The foot, calf, and thigh muscle pumps are estimated to account for approximately 90% of venous return from the lower extremities, which makes regular leg movement important for lower-body fluid dynamics. [Journal of Vascular Surgery]
How can restrictive garments worsen local fluid pressure?
Restrictive garments can worsen local fluid pressure when tight bands or compressed fabric create repeated pressure over already congested or cellulite-prone tissue. Items like very tight waistbands or rigid skinny jeans apply unyielding external force across the skin surface.
This constriction may mechanically limit shallow fluid movement, especially when sitting for prolonged periods. In some individuals, this clothing friction may worsen temporary indentation, swelling, or discomfort.
What myths should be avoided when trying to flush out localized adipose toxins?
Myths should be avoided when trying to flush out localized adipose toxins because cellulite is not caused by trapped toxins, and fluid-related cellulite visibility cannot be solved by dehydration-focused detox products. The beauty industry frequently exploits the concept of fluid retention to market ineffective cleanses.
These marketing tactics entirely misunderstand how the hypodermis handles biological waste and tissue fluid. Focusing on these myths distracts patients from genuine, supportive circulatory habits.
Why don’t detox teas correct hypodermal lymphatic stagnation?
Detox teas do not correct hypodermal lymphatic stagnation because they do not mechanically improve lymphatic drainage or remodel the connective tissue architecture that shapes cellulite visibility. Many of these teas act through simple diuretic or laxative effects, removing overall body water rather than targeting localized tissue fluid.
This temporary water loss is completely distinct from improved microvascular flow. Using the word “toxins” to describe normal interstitial fluid is a marketing myth designed to sell products.
Why can hydration alone not fix cellulite-related fluid stagnation?
Hydration alone cannot fix cellulite-related fluid stagnation because tissue fluid movement depends on lymphatic drainage, muscle activity, vascular function, and connective tissue pressure, not water intake alone. Drinking adequate water supports normal, healthy physiology across the entire body.
However, forcing excess water consumption does not act as a pressure washer that drains tissue fluid from the thighs. Real circulatory support relies heavily on movement, non-restrictive clothing, and sometimes clinician-guided care if swelling is highly significant.
Which clinical procedures may support deep tissue perfusion and drainage?
Clinical procedures may support deep tissue perfusion and drainage by mechanically mobilizing tissue, applying controlled compression, or using heat-based methods that influence local blood flow and collagen remodeling. These interventions do not guarantee a permanent cure, but they may assist sluggish fluid systems temporarily.
Depending on the device, treatments either mechanically assist the lymphatic return or thermally stimulate local blood vessels. Patient selection and clinician guidance ensure these procedures are used safely and effectively.
How can mechanical lymphatic drainage and compression support fluid movement?
Mechanical lymphatic drainage and compression can support fluid movement by applying external pressure patterns that encourage tissue mobilization and lower-body fluid return. Treatments like Endermologie use motorized rollers to gently manipulate the skin, which may temporarily support localized fluid clearing.
Similarly, pneumatic compression devices apply controlled, intermittent pressure to assist lymphatic flow in selected contexts. An evidence-based cellulite review found that only 19 of 67 analyzed studies were placebo-controlled randomized studies, which supports cautious wording for mechanical and aesthetic cellulite treatments. [PubMed]
How can radiofrequency support local circulation and dermal remodeling?
Radiofrequency may support local circulation and dermal remodeling by heating tissue in a controlled way, which can influence blood flow, collagen behavior, and temporary skin firmness. This energy-based devices tighten dermal tissue application induces thermal vasodilation, widening the local blood vessels.
This temporary heating can slightly improve local perfusion while simultaneously encouraging collagen support. A radiofrequency cellulite study reported cellulite reduction with ultrasound monitoring, but this should be framed as treatment-specific appearance improvement rather than permanent circulation restoration. [PubMed]
| Procedure | Primary Mechanism | Blood Flow vs. Lymph Focus | Clinical Efficacy Language |
|---|---|---|---|
| Manual lymphatic drainage | Gentle directional pressure | Lymph focus | May support fluid movement; not cellulite removal |
| Endermologie / mechanical massage | Rollers and suction mobilize tissue | Lymph and tissue mobilization | May temporarily improve appearance; evidence varies |
| Pneumatic compression | Intermittent external pressure | Fluid return focus | Useful for selected edema/lymphatic contexts; clinician-guided |
| Radiofrequency | Controlled tissue heating | Blood flow and collagen support | May improve firmness/appearance in selected patients |
| Exercise / walking | Muscle-pump activation | Venous and lymphatic return | Practical daily support habit |
| Leg elevation | Gravity-assisted fluid redistribution | Fluid pooling support | Temporary relief, not structural cellulite treatment |
What daily checklist helps maintain healthy subcutaneous fluid dynamics?
A daily checklist helps maintain healthy subcutaneous fluid dynamics by combining movement, gentle tissue handling, non-restrictive clothing, hydration, and realistic expectations about cellulite appearance. Practical fluid management requires consistent, mild supportive habits rather than extreme interventions.
This approach actively minimizes the lifestyle triggers that worsen lower-body congestion. Adopting these non-invasive steps preserves tissue comfort and slightly improves visual texture over time.
How can mechanical pumping habits support lower-body fluid movement?
Mechanical pumping habits can support lower-body fluid movement by using leg muscle contractions to help venous blood and lymphatic fluid return from dependent tissues. Small activities like calf raises, taking the stairs, or light cycling engage these essential muscular pumps.
A practical routine can include a 2-minute walking break every hour, serving as a helpful behavioral suggestion rather than a medically required threshold. Avoid aggressive dry brushing, favoring only gentle massage if it feels comfortable.
How can posture and environment reduce fluid pooling?
Posture and environment can reduce fluid pooling by limiting prolonged static positions, avoiding restrictive pressure points, and using brief leg elevation when lower-leg heaviness or swelling is present. Standing or walking breaks break the cycle of static pooling.
Elevating the legs for 15 minutes can be presented as a practical comfort habit to ease daily swelling. However, any sudden, painful, or unexplained one-sided swelling requires immediate clinician review.
Daily Hypodermal Microcirculation & Drainage Checklist
FAQs About Circulation in Cellulite-Affected Hypodermal Tissue
Does cellulite mean circulation is blocked?
No. Cellulite does not mean circulation is fully blocked. Cellulite-affected tissue may show less efficient microcirculation, altered lymphatic drainage, and fluid imbalance, but this should be framed as a tissue-flow issue rather than a complete vascular blockage.
Does poor lymphatic drainage cause cellulite?
Poor lymphatic drainage may contribute to fluid retention and visible swelling, but it is not the only cause of cellulite. Cellulite also involves fibrous septae, fat lobules, dermal support, hormones, genetics, and tissue architecture.
Can sitting make cellulite look worse?
Prolonged sitting may make cellulite look more noticeable by reducing leg muscle-pump activity and fluid return. The foot, calf, and thigh muscle pumps are estimated to account for about 90% of lower-extremity venous return.
Do detox teas flush cellulite toxins?
No. Detox teas do not flush cellulite toxins because cellulite is not caused by trapped toxins. These products may change body water temporarily, but they do not remodel fibrous septae, restore microcirculation, or correct hypodermal tissue architecture.
Can drinking more water fix cellulite circulation?
Hydration supports normal physiology, but drinking more water alone does not correct cellulite-related tissue architecture. Fluid movement depends on lymphatic drainage, muscle activity, vascular function, connective tissue pressure, and overall health.
Does massage improve cellulite circulation?
Massage may temporarily support tissue mobilization, local comfort, or fluid movement, but it should not be presented as a permanent cellulite cure. Aggressive massage can irritate or bruise sensitive skin, so pressure should stay gentle and tolerable.
Which treatments target circulation or drainage most directly?
Mechanical massage, Endermologie-style tissue mobilization, pneumatic compression, and radiofrequency may target fluid movement or local tissue response. Evidence varies, and an evidence-based review found only 19 of 67 analyzed cellulite studies were randomized placebo-controlled studies.
Conclusion
Circulation in cellulite-affected hypodermal tissue can become less efficient when fat lobules, fibrous septae, fluid pressure, and reduced movement interfere with blood flow and lymphatic drainage. This flow change may contribute to swelling, tissue stiffness, and more visible dimpling, but it should not be framed as a toxin problem or complete vascular blockage.
At SkinKeeps, we explain cellulite through evidence-based skin structure and physiology. Understanding hypodermal circulation helps readers choose realistic habits and clinician-guided treatments with calm, informed expectations.