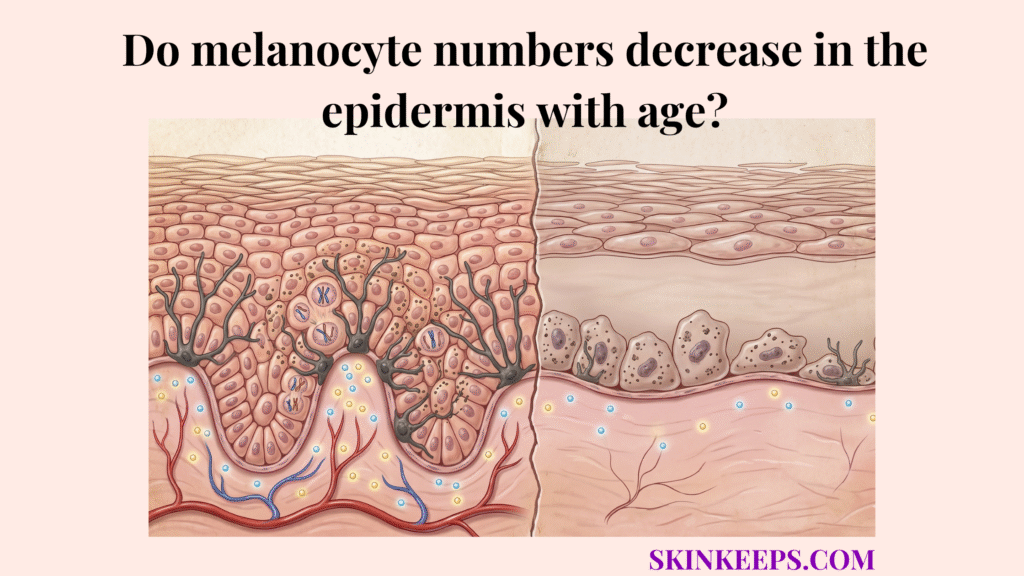
Yes, melanocyte numbers generally decrease in the epidermis with age. As these pigment-producing cells become fewer and less evenly distributed over time, the skin’s pigment response, UV protection, and color uniformity often change as well.
Explain that this decline does not always create simpler or lighter-looking skin. Even when melanocyte numbers decrease, the remaining cells may behave less evenly, and long-term sun damage can make pigmentation look more patchy rather than more uniform.
Understanding age-related epidermal melanocyte decline makes it easier to explain what changes first, how pigment behavior shifts, why uneven tone often increases with age, and what helps preserve healthier pigment stability.
What begins first in age-related epidermal melanocyte decline?
Age-related epidermal melanocyte decline usually begins as a slow reduction in melanocyte density before obvious visible changes appear. Age-related epidermal melanocyte decline—the gradual reduction and destabilization of melanocyte support in aging epidermis—directly impacts the melanocyte (the pigment-producing cell located mainly in the basal epidermis) and overall melanocyte density, which refers to how many melanocytes are present within a given epidermal area.
The change may develop slowly before tone differences become easy to notice, and that early decline is often more about reduced cellular reserve than sudden pigment loss.
Rittié and Fisher, 2015 describe aging skin as showing about a 10% to 20% reduction in melanin-producing melanocytes per decade after around age 30, which supports the idea that melanocyte decline is gradual and cumulative rather than abrupt (Rittié and Fisher, 2015).
How does reduced cell density drive age-related epidermal melanocyte decline?
Reduced cell density drives age-related epidermal melanocyte decline because fewer pigment-producing cells are available to maintain balanced epidermal melanin support.
The epidermis depends on an adequate melanocyte population to maintain steady pigment coverage, and when melanocyte density falls, pigment production becomes less evenly supported across the skin.
This can reduce baseline pigment consistency and weaken photoprotective uniformity, especially when the remaining melanocytes are no longer distributed as evenly as before.
How does age-related epidermal melanocyte decline change melanin production and transfer?
Age-related epidermal melanocyte decline changes melanin production and transfer by making pigment output less evenly distributed across the epidermis. Melanin transfer is the movement of pigment from melanocytes into surrounding keratinocytes.
Melanocytes do not only produce pigment; they also transfer it to surrounding keratinocytes, so lower melanocyte support changes both output and distribution.
When melanocyte numbers decline, pigment production and distribution become less consistent, which can contribute to irregular tone, reduced evenness, and altered UV-response patterns.
How does UV exposure accelerate age-related epidermal melanocyte decline?
UV exposure accelerates age-related epidermal melanocyte decline by increasing cumulative cellular stress and making pigment behavior less even over time.
UV exposure adds repeated stress to melanocytes over time, which can reduce melanocyte stability and contribute to cumulative cellular loss.
Gilchrest, Blog, and Szabo, 1979 reported that melanocyte density was roughly twofold higher in habitually sun-exposed skin than in adjacent protected skin at all ages, yet melanocyte density still declined by about 6% to 8% of the surviving population per decade in both sites. That helps explain why fewer melanocytes do not automatically create more even skin tone; photoaged skin can still look blotchier because the remaining cells behave more irregularly (Gilchrest, Blog, and Szabo, 1979).
How does chronic UV stress worsen age-related epidermal melanocyte decline?
Chronic UV stress worsens age-related epidermal melanocyte decline by adding repeated damage pressure to melanocytes that are already becoming fewer and less stable over time.
This repeated stress can reduce melanocyte stability and contribute to cumulative cellular loss.
Long-term exposure often makes age-related decline more visible and more irregular.
How does photodamage distort pigment patterns during age-related epidermal melanocyte decline?
Photodamage distorts pigment patterns during age-related epidermal melanocyte decline because fewer melanocytes do not always produce simpler pigmentation.
Sun-damaged skin may show uneven activity among the remaining cells, which helps explain why aging skin can look both thinner in pigment reserve and more blotchy in tone.
Reduced cell count and irregular pigment expression can coexist.
How does age-related epidermal melanocyte decline weaken epidermal photoprotection?
Age-related epidermal melanocyte decline weakens photoprotection by reducing the consistency and reserve of melanin-based UV defense. Photoprotection is the skin’s ability to reduce some UV-related damage through pigment and other defenses.
Melanin helps absorb and redistribute some UV stress, so when melanocyte numbers decrease the epidermis may lose part of its pigment-based protective reserve.
This can leave aging skin less evenly defended against further photodamage because melanin support becomes less consistent across the epidermis.
Which signs suggest age-related epidermal melanocyte decline is becoming more visible?
Age-related epidermal melanocyte decline may be becoming more visible when skin tone looks more patchy, less uniform, and less predictably responsive to sun or inflammation.
Warning signs can include more uneven skin tone, greater contrast between lighter and darker areas, increased mottling or patchiness, slower recovery after pigment-triggering inflammation, and reduced color consistency across chronically sun-exposed areas.
These visible changes reflect less stable pigment support rather than simply “more pigment” or “less pigment” everywhere.
How does youthful melanocyte distribution compare with age-related epidermal melanocyte decline?
Youthful melanocyte distribution is denser and more even, while age-related epidermal melanocyte decline reduces pigment stability and makes tone less uniform.
Youthful epidermis maintains higher and more stable melanocyte support, which helps keep pigment distribution and photoprotective behavior more balanced.
Age-related decline lowers that reserve and makes pigment maintenance less even over time.
| Pigment state | Melanocyte density | Pigment distribution | Tone uniformity | Photoprotective consistency |
|---|---|---|---|---|
| Youthful epidermis | Higher and more stable | More even | More uniform | More balanced |
| Age-related epidermal melanocyte decline | Lower and less stable | Less even | More patchy | Less consistent |
How does age-related epidermal melanocyte decline differ from irregular melanocyte overactivity?
Age-related epidermal melanocyte decline differs from irregular melanocyte overactivity because one describes fewer cells overall, while the other describes uneven behavior among the cells that remain.
A decline in melanocyte numbers does not automatically mean less visible pigmentation everywhere.
Remaining melanocytes may become uneven in behavior, especially in photoaged skin, which is why reduced cell count and irregular pigment expression can coexist.
What factors make age-related epidermal melanocyte decline worse?
Age-related epidermal melanocyte decline worsens when cumulative damage and chronic sun stress outpace the skin’s ability to preserve stable pigment-cell function.
Common worsening factors include chronic UV exposure, repeated photodamage, ongoing oxidative stress, chronic inflammation, poor daily photoprotection, and ignoring early pigment instability in aging skin.
These factors deepen decline by increasing stress on the remaining melanocyte system rather than by simply darkening the skin uniformly.
What habits and ingredients help support skin affected by age-related epidermal melanocyte decline?
The best support for skin affected by age-related epidermal melanocyte decline combines consistent photoprotection, lower inflammation, and routines that preserve pigment stability rather than provoking it.
The goal is not to force pigment correction aggressively. The goal is to protect remaining melanocyte function and reduce the stress that makes pigment behavior more unstable.
This guides the approach for the targeted protective steps below.
How does sun protection help support skin affected by age-related epidermal melanocyte decline?
Sun protection helps support skin affected by age-related epidermal melanocyte decline by reducing further UV-driven melanocyte stress.
Daily SPF helps protect the pigment reserve that remains and lowers the chance of worsening visible unevenness.
Consistent photoprotection is the single most important long-term support habit for this pattern.
How does barrier support help skin affected by age-related epidermal melanocyte decline?
Barrier support helps skin affected by age-related epidermal melanocyte becahse amore stable barrier reduces inflammatory stress that can worsen pigment irregularity.
Lower irritation helps reduce secondary pigment instability.
This supports more balanced skin behavior overall.
How do gentle pigment-supportive routines help skin affected by age-related epidermal melanocyte decline?
Gentle pigment-supportive routines help skin affected by age-related epidermal melanocyte decline by reducing unnecessary inflammatory triggers and preserving steadier epidermal function.
Avoiding over-exfoliation and chronic irritation helps preserve steadier pigment behavior over time.
More stable skin often shows more stable visible tone.
Problem: age-related epidermal melanocyte decline is increasing
Implication: pigment support and tone uniformity are becoming less stable
Solution: protect from UV, reduce inflammatory stress, and support barrier stability
What are the key takeaways about age-related epidermal melanocyte decline?
Melanocyte numbers generally decrease in the epidermis with age, and this decline makes pigment support less even over time.
To protect long-term tone quality, preserving the existing cellular environment through lower stress is essential.
Summary Points
- Melanocyte numbers generally decrease in the epidermis with age.
- This decline reduces pigment-cell density and makes melanin support less even over time.
- UV exposure and chronic stress can accelerate the decline and worsen pigment irregularity.
- Fewer melanocytes do not always produce more even skin tone; they often contribute to less stable pigment distribution.
- The best support strategy focuses on sun protection, barrier stability, and lower inflammatory stress.
FAQs About Age-Related Epidermal Melanocyte Decline
Do melanocyte numbers decrease in the epidermis with age?
Yes. Melanocyte numbers usually decline gradually with age, so the epidermis has fewer pigment-producing cells available over time.
Does fewer melanocytes mean skin tone becomes more even?
No. Fewer melanocytes do not automatically create more even skin tone. The remaining melanocytes may behave less evenly, which can make the skin look more patchy instead of more uniform.
Why can aging skin look blotchy if melanocyte numbers are falling?
Because age-related epidermal melanocyte decline can happen alongside irregular pigment behavior in the melanocytes that remain, especially in sun-damaged skin.
Does age-related epidermal melanocyte decline reduce photoprotection?
Yes. Melanocytes help support melanin-based UV defense, so when their numbers decline, pigment-based photoprotection can become less even across the epidermis.
What helps support skin affected by age-related epidermal melanocyte decline?
Daily broad-spectrum SPF, barrier-supportive skin care, and gentle low-irritation routines help protect the melanocytes that remain and support more stable visible tone.
What daily steps help reduce the impact of age-related epidermal melanocyte decline?
Daily steps help reduce the impact of age-related epidermal melanocyte decline by protecting the melanocytes that remain and lowering the stress that makes their behavior more unstable.
Long-term pigment stability depends more on consistency and lower stress than on aggressive corrective routines.
Daily Pigment Stability Checklist
Age-related epidermal melanocyte decline does not only reduce cell numbers. It changes how evenly pigment is maintained across the epidermis.
Build your routine around photoprotection, barrier support, and lower inflammatory stress if your goal is steadier tone and healthier aging skin.